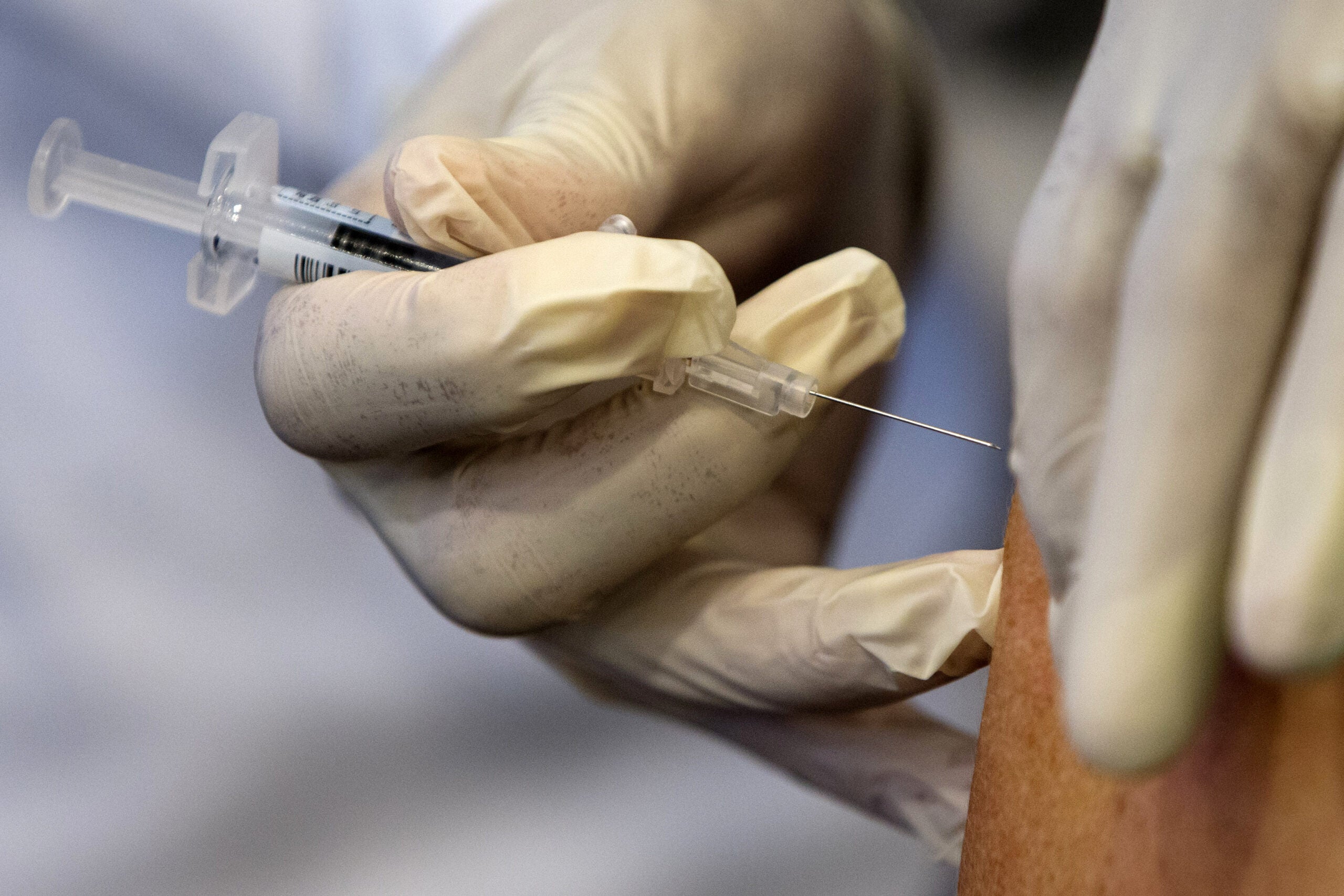
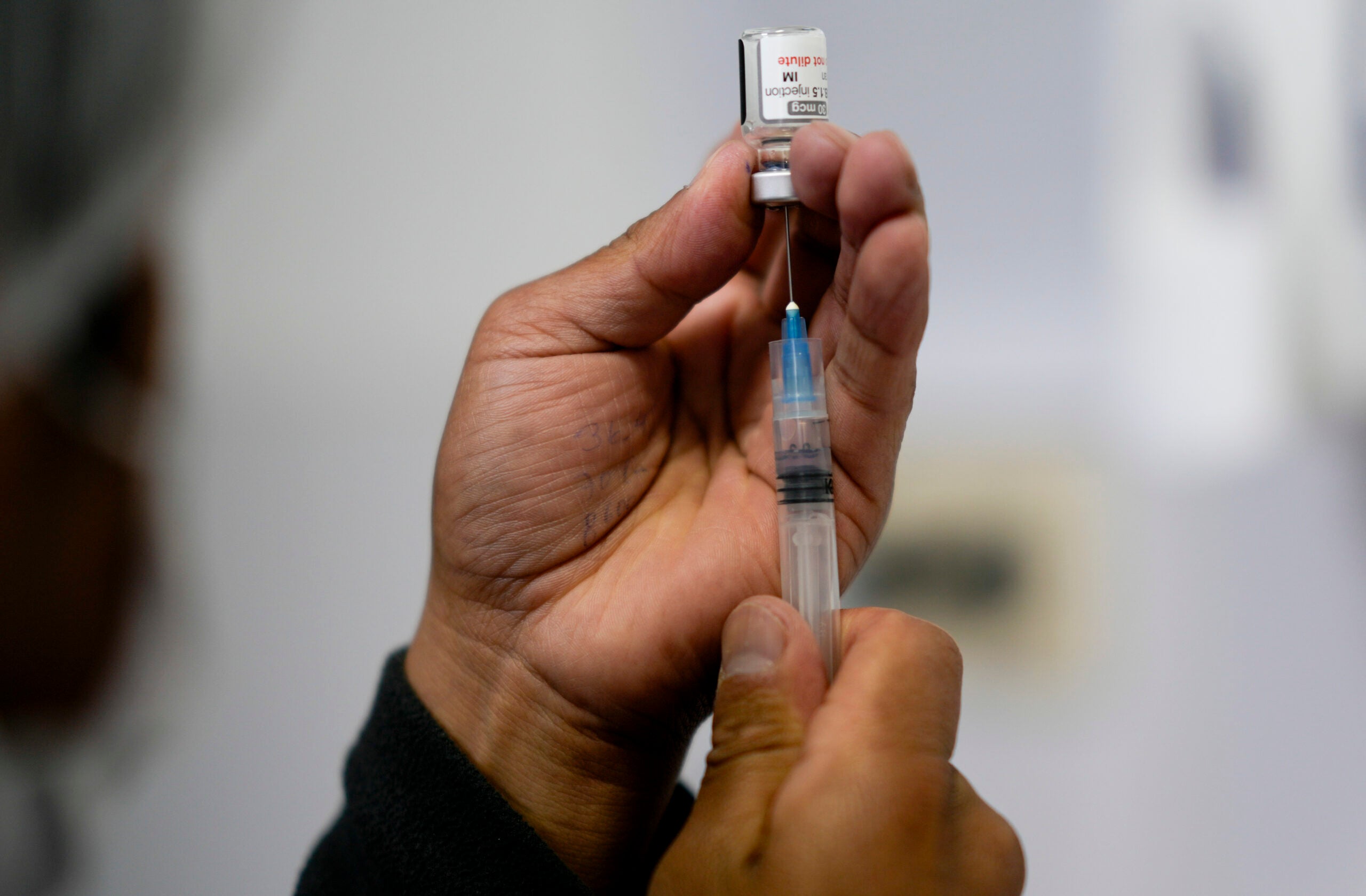
Some have called a coronavirus vaccine “salvation in a syringe.” It can’t come soon enough for Dr. Neil Bard, who still remembers the fear of polio during an outbreak in the 1950s.
“People got paralyzed from polio,” he recalled. “I remember being taken by my parents — rushed — to the local elementary school, and we couldn’t wait for the public nurse to vaccinate us.”
Bard, the medical director at Richland Hospital Clinic in southwestern Wisconsin, has been on guard since the coronavirus made its way to the state.
News with a little more humanity
WPR’s “Wisconsin Today” newsletter keeps you connected to the state you love without feeling overwhelmed. No paywall. No agenda. No corporate filter.
“We have to be vigilant,” he said. “We have to watch for any type of increase (in COVID-19 cases) that might overwhelm our ability to care for people.“
Public appeals by Wisconsin’s current and former governors to “smash” the coronavirus or “box it in,” have been stymied by an inactive state Legislature and a disregard among many residents for public health recommendations.
But with a vaccine on the horizon, there’s hope that medicine will finally bring an end to the pandemic that has claimed the lives of more than 3,800 Wisconsinites. The coronavirus vaccine, though, won’t be in widespread use until spring or summer. And hospitals across the state are bracing for what winter could bring as people gather to celebrate the holidays and cold weather moves people indoors.
Clamoring For A COVID-19 Vaccine
The success rate and speed at which several coronavirus vaccines have been developed has been called remarkable — the scientific achievement enabled by technological advancements not around when other older vaccines were created.
“We’re in a different age now where we have machine learning, artificial intelligence. All this can unlock the genome much, much faster than when they were trying to create a vaccine for polio or the measles,” said Lisa Johnson, CEO of BioForward Wisconsin. The trade group promotes the growth of the state’s biotech companies, some of which were involved in the manufacture of COVID-19 tests and treatments.
Daunting challenges lie ahead, however: mass production and distribution of the vaccine, and persuading the public to take it. Three former U.S. presidents have said they’re willing to publicly get the coronavirus vaccine. And a recent poll by the Pew Research Center found that 60 percent of Americans said they would get vaccinated.
But every year the United States falls short of its goal of convincing 70 percent of Americans to get a seasonal flu shot.
So far this flu season, 37 percent of people in Wisconsin have been vaccinated against influenza, according to a weekly update from the state Department of Health Services. That’s despite a strong effort to get people vaccinated this year so hospitals aren’t overwhelmed with both COVID-19 and flu cases.
Last year, 42 percent of Wisconsin resident were vaccinated against the flu.

At Richland Hospital Clinic, Bard said more flu vaccines have been given this year than ever before, and he’s optimistic people will accept vaccines against the coronavirus.
“I’m hoping it’s going to be like the polio vaccine that people will be clamoring for this. I already have patients who I give the flu shot to and they say, ‘Tell me when ‘the big one’ is here because I want it,” he said.
‘The Last Line Of Defense’
Before that can happen, though, Wisconsin needs to make it through the winter. When the state’s COVID-19 surge was at its worst in November, hospitals around the state made use of their surge plans. They made extra space for beds, treating those with milder COVID-19 symptoms at home, and relying on each other to take patients they can’t care for. Even before the pandemic, smaller hospitals routinely transferred patients to bigger hospitals that can provide more advanced care. But now even small hospitals are getting requests to take additional patients as beds fill up across the state.
Richland Hospital, which only has 20 beds, was even asked to accept a patient from a larger hospital.
“We were pretty surprised to get a call from Watertown (Regional Medical Center) which is two hours away,” Richland Hospital Chief of Staff Dr. Christine Richards told WRCO radio. “I’m sure they typically would use either Madison or Milwaukee as their referral. That indicates to us that hospitals around the state are starting to reach capacity and having trouble finding places for their COVID-19 patients to be cared for.”
Staff at Richland Hospital advised Watertown Regional Medical Center to seek care for the patient elsewhere, a decision Bard said was “to protect our staff from exhaustion.”
In western Wisconsin, St. Croix Regional Medical Center had to transfer a severely ill patient to Fargo, North Dakota — 272 miles away — because hospitals in the Twin Cities were at capacity. Sometimes it’s lack of a bed. Often, it’s not enough staff.
“There is a current sense in health care that the hospitals and clinics — which were once the front line for our war against COVID-19 — are now the last line of defense,” said Dr. Ruth Smith, a family medicine physician at SCRMC. “The current war is being fought in our communities, and we need participation from everyone to try to save as many lives as we can.”

Hospitalizations in Wisconsin peaked on Nov. 17 with 2,277 patients. Since then, hospitalizations have declined for both regular and ICU beds. A similar trend has been seen in other states, but some doctors warn it may be an issue of capacity, not the level of care needed.
That’s why Wisconsin hospitals pleaded with the public in late September to “buckle down” and get serious about a virus that some claim is no worse than the flu. While many cases are mild, more than a dozen people have died from the virus in Richland County since the pandemic began.
Richland County’s largest city and county seat — Richland Center — is home to just over 5,000 people. The county itself has a population of roughly 17,250 people. Like many small towns in the Midwest, people greet each other warmly at the gas station and vehicles stop for pedestrians even when there’s no stop sign or crosswalk. But the common-good act of mask-wearing during a pandemic has been caught up in politics and disbelief in its efficacy, Bard said.
“I think that sometimes people think because it’s not some miraculous drug or injection or something high-tech, it can’t be worthwhile,” he said. “But we’ve learned since the spring that this a major way to take care of this pandemic.”
Health Care Professionals Plead For Vigilance
Deaths have increased sharply in recent months from COVID-19. It’s taken a tremendous toll on health care workers. Dr. Talha Khan, a pulmonary medicine doctor and chief of staff at St. Croix Regional Medical Center, recalls a particularly difficult situation where an elderly patient endured a serious medical condition, interstitial lung disease, for years only to die after becoming infected with the coronavirus.

“I still cannot shake the sadness. We were able to manage her significant underlying disease for four years which is difficult to do, however, I lost the patient to COVID-19, a preventable disease” said Khan.
The woman’s husband, also sick with COVID-19, was in another room at the hospital. When his wife’s condition worsened, staff wheeled him to her room so they could be together before she died.
Many doctors fear an increase in preventable deaths, as people’s resolve seems to be weakening.
“The problem is we did a better job of it early on when we had almost no cases in this county,” Bard told WRCO radio “Now we are essentially overrun, just like the rest of the state. We’ve got people who are tired of this. We can’t be tired of this. We have to be vigilant and we have to use the tools that we have.”
WRCO general manager Ron Fruit describes Bard, who is also his personal physician, as “a voice of reason” who makes regular appearances on local radio to dispel myths and promote behavior to reduce spread of the coronavirus.
Even with the finish line in sight, the last stretch of a long race can be the most difficult. Health professionals say people still have to keep their guard up against a virus that shows no signs of letting up. And national health officials have warned that the most brutal period of the pandemic lies ahead: the period when infections are still spreading and the vaccine isn’t yet widely available.
Wisconsin Public Radio, © Copyright 2026, Board of Regents of the University of Wisconsin System and Wisconsin Educational Communications Board.