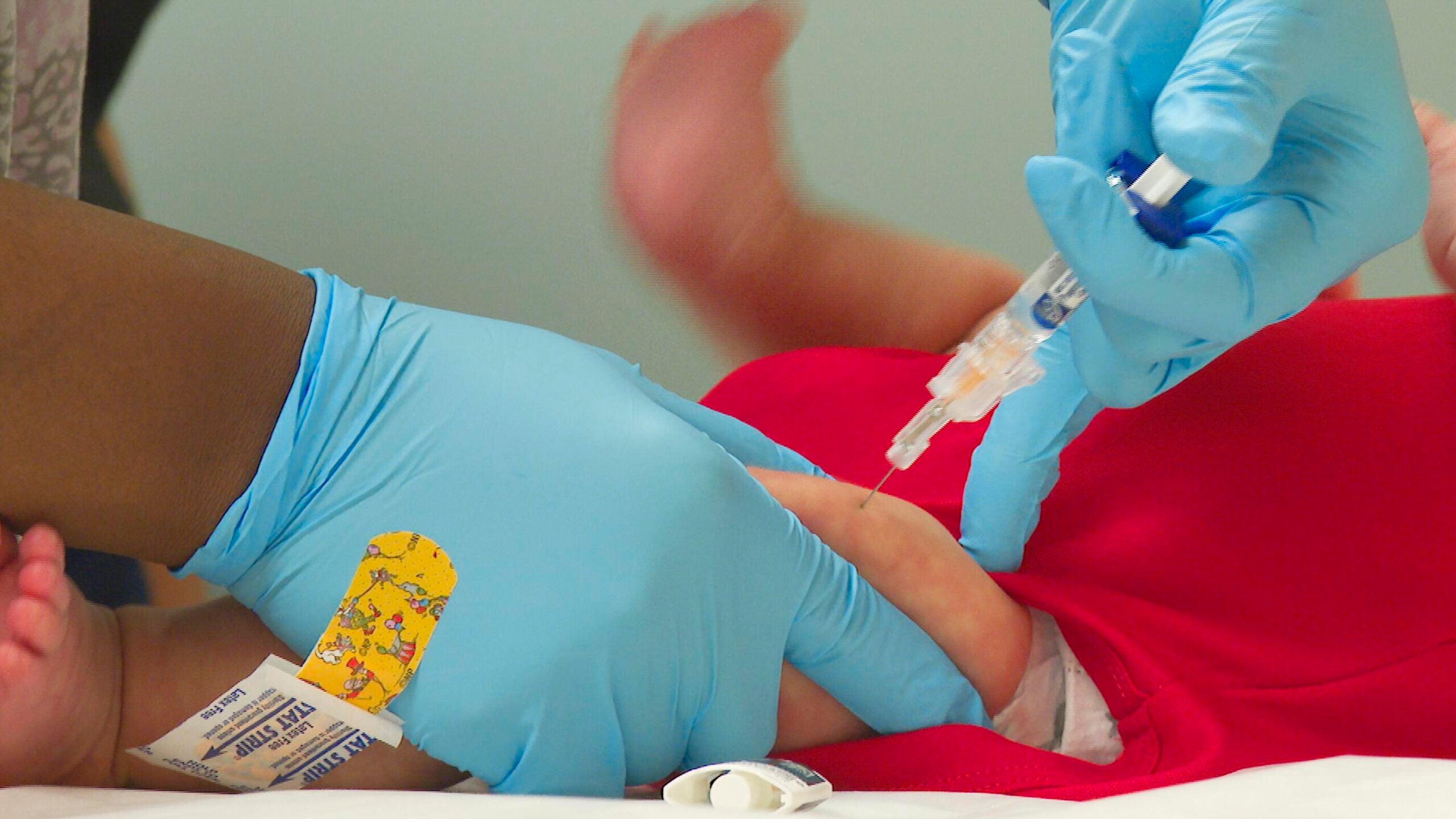
The new coronavirus has moved like a wave across communities in Wisconsin. First growing rapidly in Milwaukee County in March, and then working its way to other parts of the state.
In April, Brown County was hit with hundreds of COVID-19 cases after two meatpacking plants had employees test positive.
Now, Kenosha and Rock counties are two of the latest areas of the state to see a surge.
News with a little more humanity
WPR’s “Wisconsin Today” newsletter keeps you connected to the state you love without feeling overwhelmed. No paywall. No agenda. No corporate filter.
In Kenosha County there were 627 confirmed cases of COVID-19 as of May 8 and 15 people have died, according to the state Department of Health Services (DHS).
There were 343 confirmed cases of COVID-19 in Rock County as of May 8 and 12 people have died, according to DHS.
The rate of positive coronavirus cases as of May 8 in Kenosha County is 373 per 100,000 people and in Rock County it’s 212 per 100,000 people, according to DHS.
By comparison, the rate is 27 per 100,000 people in La Crosse County; 86 per 100,000 people in Dane County; 390 per 100,000 people in Milwaukee County and 684 per 100,000 people in Brown County.
Officials with the Rock County Health Department could not be reached for comment. In an email to The Janesville Gazette, Rick Wietersen, environmental health director for the department, said the reason for the increased cases was two-fold. Many of the positive cases came from residents who work at Birds Eye food processing plant in Walworth County and more people are now being tested.
Dr. Ben Weston, medical director of the Milwaukee County Office of Emergency Management, said it’s no secret there was a great shortage of tests on a national scale.
Testing capacity is starting to increase and now, anyone who is symptomatic is being told to get tested.
“People with symptoms have been waiting to be tested so there is going to be an unofficial surge,” Weston said. “It’s a little hard to get the lay of the land to get what the COVID-19 tests are because we have more tests out. I think we’ll reach, very soon, another steady state of what trend we are on.”
This Is Not The Flu
Weston said the patchwork nature of the virus can be traced to how the virus spreads compared to other highly contagious illnesses like Influenza, which can also be transmitted via contact and in droplets.
On average, a person who is infected with influenza, typically infects about 1.2 people, Weston said. By comparison, a person infected with COVID-19 infects two to three people.
“That doesn’t sound like that big of a difference, but if you go to five generations of spread (of COVID-19), soon you’ve got 30 people who are sick,” Weston said.
Another difference is a person is most contagious with COVID-19 while they are asymptomatic, and they can have the virus for up to 14 days without knowing it. Whereas a person with influenza is most contagious when they have symptoms from the virus and are already at home.
“With COVID-19 you might be feeling fine, you might be interacting with people,” Weston said. “Every time you breathe, every time you talk, and certainly every time you cough or sneeze, droplets are coming out of your mouth and you are infecting people.”
Dr. Nasia Safdar, medical director of infectious disease control at UW Health, said because people are asymptomatic and spreading the coronavirus, there is no way to stop the spread of the COVID-19 without screening and testing hundreds of people before they get sick.
“I think that is one reason we are not seeing an entire region, or a particular large region at one time,” Safdar said.
Population density is also a factor.
“So when people are close together and there is no way to distance yourself, that is where we see the big cluster and then that cluster … cascades out toward the rest of the community,” Safdar said.
Looking Ahead
As the state slowly begins to reopen, either with a directive from the state Supreme Court of through Gov. Tony Evers administration’s “Badger Bounce Back plan“, Safdar said it’s inevitable there will be more cases of the coronavirus.
But, she said, we can’t go on living in seclusion forever.
Instead, Safdar suggests opening slowly, limiting travel and not holding large public gatherings — which will have to be a “new normal” until a vaccine is developed.
“Some less restrictive approach to what is happening now, just because we can’t keep living this way forever, but not going back wholesale to the way of life that we had before,” Safdar said. “It’s a very complicated situation.”
Wisconsin Public Radio, © Copyright 2026, Board of Regents of the University of Wisconsin System and Wisconsin Educational Communications Board.