A second coronavirus vaccine could be approved soon by federal regulators, paving the way for Wisconsin to receive 100,000 doses of the Moderna vaccine as early as next week.
That would increase Wisconsin’s limited stockpile and is twice what the state received in its initial shipment of nearly 50,000 doses from Pfizer.
The first vaccines come less than a year after Wisconsin confirmed its first case of COVID-19.
News with a little more humanity
WPR’s “Wisconsin Today” newsletter keeps you connected to the state you love without feeling overwhelmed. No paywall. No agenda. No corporate filter.
“This is a really exciting moment. It’s really critical to be entering this phase of our response to the pandemic,” said Wisconsin Department of Health Services Secretary Andrea Palm on Tuesday.
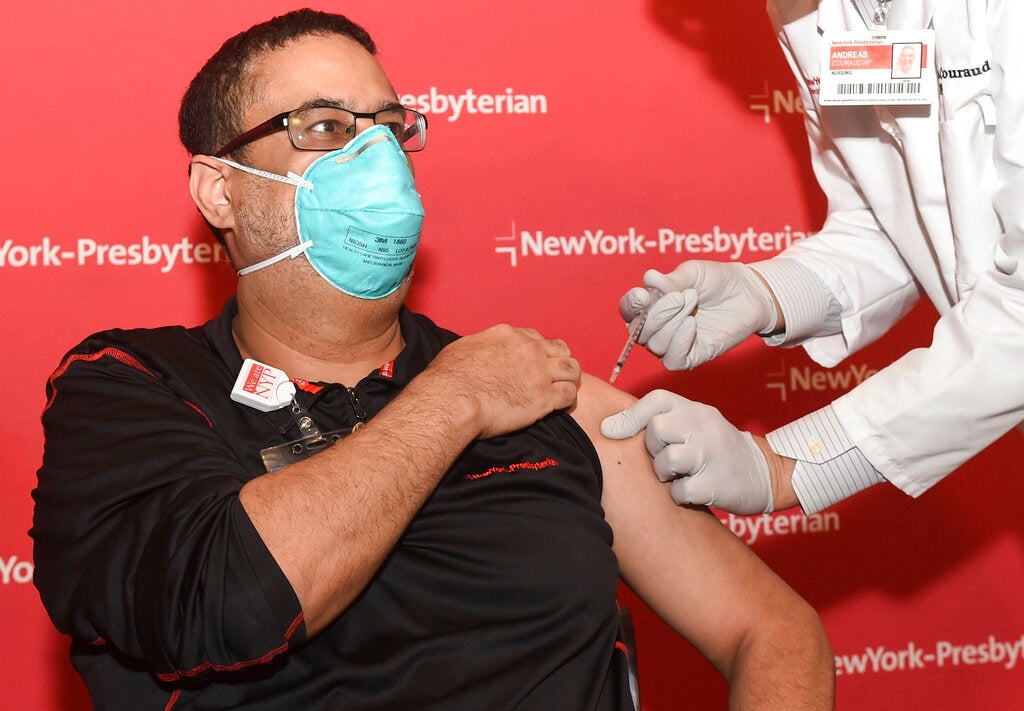
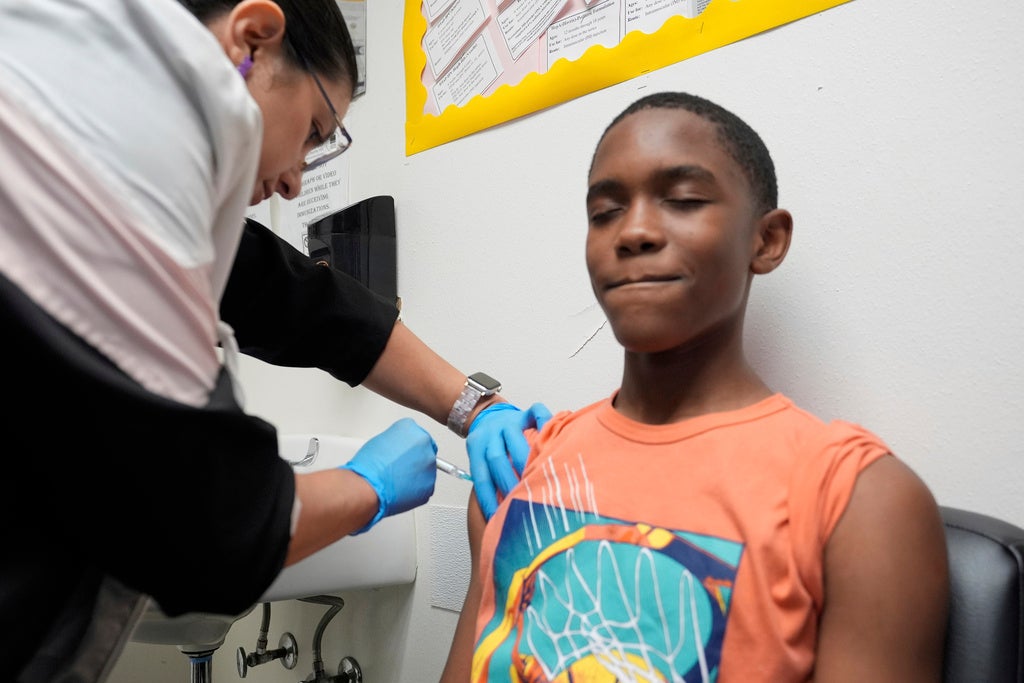
Frontline health care workers started receiving doses of the vaccine Monday. Another priority group is people in long-term care facilities.
Gov. Tony Evers announced Monday that DHS has activated a federal partnership with pharmacy chains that would distribute vaccines to long-term care facilities around the country.
Under the partnership, pharmacy chains CVS and Walgreens will administer vaccines to nursing home residents and workers. State officials hope this could be nearly complete by the end of January.
Nursing homes are going over details with DHS on when and how this will happen. Consent of long-term residents will be needed before any shots go in arms, possibly as early as Monday, Dec. 28.
“So, there’s a lot of logistical considerations that are going to have to be addressed in a two-week period,” said John Sauer, president and CEO of LeadingAge Wisconsin, a statewide association representing nursing homes, assisted living facilities and other community-based providers in the state.
Once pharmacy chains get the vaccine from the federal government, they will set up inoculation timetables for each facility in Wisconsin.
Sauer said there are approximately 28,000 long-term care residents and at least that many staff.
“What we don’t know is how many staff or residents elect not to receive the vaccine,” Sauer said.
Suffering caused by the disease, which has resulted in the deaths of many older adults, might convince workers and residents to be vaccinated.
“They know that this could literally be a life-and-death situation,” Sauer told Modern Healthcare, which said no reliable gauges of nursing home residents’ opinion on the vaccine have emerged.
In public comments to state health officials regarding vaccine allocation, Sauer stressed that most facility outbreaks have been traced to staff bringing the virus into facilities through community contacts.
“Having our facility staff vaccinated as soon as possible will increase our ability to protect the vulnerable populations we serve,” he wrote.
For every 100 residents in nursing homes, two died during a four-week period ending Nov. 15, placing Wisconsin as the sixth-highest COVID-19 nursing home death rate in the country, said Robert J Kellerman, who submitted comments to state officials on behalf of the Greater Wisconsin Agency on Aging Resources.
Wisconsin Public Radio, © Copyright 2026, Board of Regents of the University of Wisconsin System and Wisconsin Educational Communications Board.