Hospitals in Wisconsin are seeing record numbers of COVID-19 patients, the consequence of weeks of unchecked spread of the pandemic across the state.
The increase has put hospitals at or above 90 percent of their capacity in some regions, and workers are putting into place surge plans they made months ago in the first stage of the pandemic, but haven’t had to use until now.
“We’re in the surge,” said Tammy Simon, the vice president of patient safety at Marshfield Clinic. “Our numbers are at an all-time high in our system.”
News with a little more humanity
WPR’s “Wisconsin Today” newsletter keeps you connected to the state you love without feeling overwhelmed. No paywall. No agenda. No corporate filter.
They are at an all-time high across the state. According to data from the Wisconsin Hospital Association, as of Thursday, 1,453 people were hospitalized with COVID-19. There were 330 patients in intensive care units, the second-highest that number has been in the pandemic following a decline from Wednesday’s total of 339 patients in the ICU.
Marshfield Clinic, a health system with hospitals in cities including Marshfield, Eau Claire and Beaver Dam, is treating about 90 patients with the disease, Simon said.
“What’s concerning to us is that previously we saw COVID patients trickle in,” she said. “Now, those numbers are doubling by the day.”
Because hospitalizations tend to lag several weeks behind new infections, the burden on hospitals across the state is likely to increase. For the first time this week, the seven-day average of new infections in the state topped 4,000 per day.
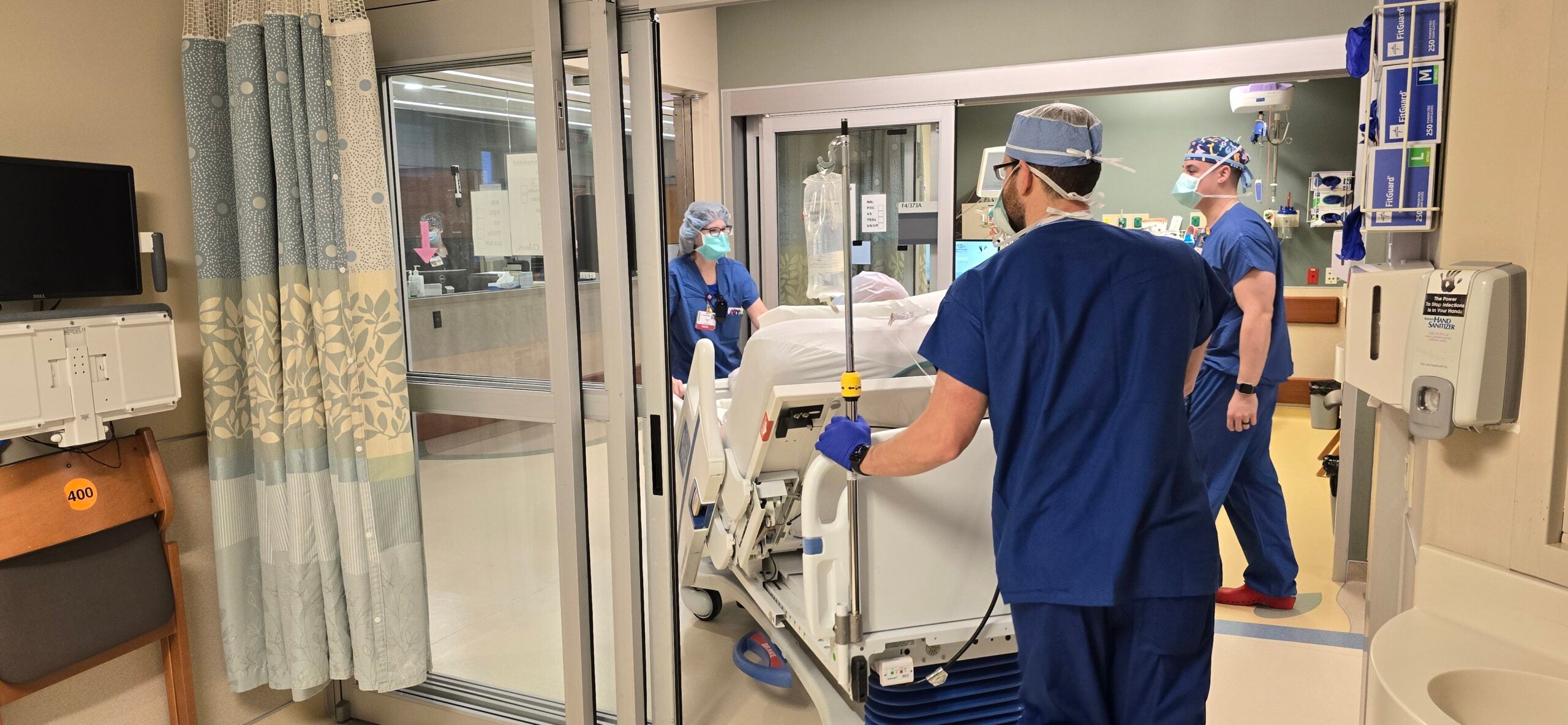
Health care workers say the physical and emotional strain on those who work in COVID-19 units is intense. Hospitals have had to make a number of adaptations: opening dedicated wards; transferring staff and patients; using telehealth visits for routine care; and delaying elective surgeries.
One effect of high community spread is that health care workers themselves contract the disease. Like other health systems across the state, Marshfield Clinic is struggling with staffing. According to state data, about 5 percent of Wisconsin’s COVID-19 cases are among health care workers. But the loss of workers at the same time patients are surging puts additional pressure on hospitals.
Simon said the fact that new infections are surging across most of the U.S. also means that it’s hard to hire nurses or other traveling staff. During New York City’s surge of cases in April, providers from across the country traveled there to help care for patients. Today, there’s no surplus of doctors and nurses to come to Wisconsin.
Fox Valley hospitals are the hardest-hit in the state. On Thursday, capacity in the region was at 93 percent. At ThedaCare, a system including hospitals in Appleton, Neenah and Shawano, chief clinical officer Dr. Mark Cockley said providers are making day-by-day decisions about how to care for COVID-19 patients while also maintaining care for others and capacity to receive patients with emergency needs not related to COVID-19.
“As the surge continues and more and more people get infected, no one has the ability to do everything,” Cockley said.
Still, some of the issues that were present early in the pandemic are no longer major challenges for hospitals. Wisconsin has enough ventilators — in part because as doctors have learned more about treating COVID-19 patients, they’ve been used less. According to WHA data, few hospitals in the state lack sufficient supplies of personal protective equipment. And most have other plans for further scaling up capacity for patient space if needed, including opening new COVID-19 units or changing how they use existing space.
Public health professionals at all levels have issued the same calls for months to slow the spread of the disease: stay home when possible, wear masks around others, maintain social distance and practice personal hygiene.
“The more we adhere to those things, the less likely we are to cause the spread,” Cockley said.
Wisconsin Public Radio, © Copyright 2026, Board of Regents of the University of Wisconsin System and Wisconsin Educational Communications Board.