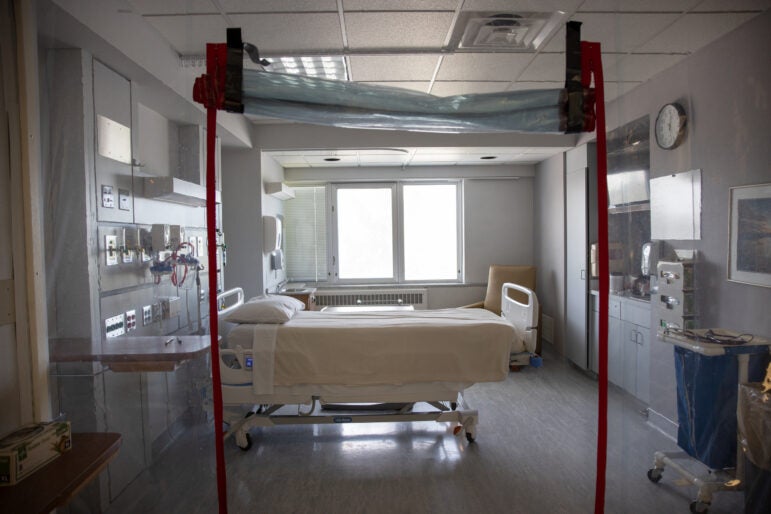
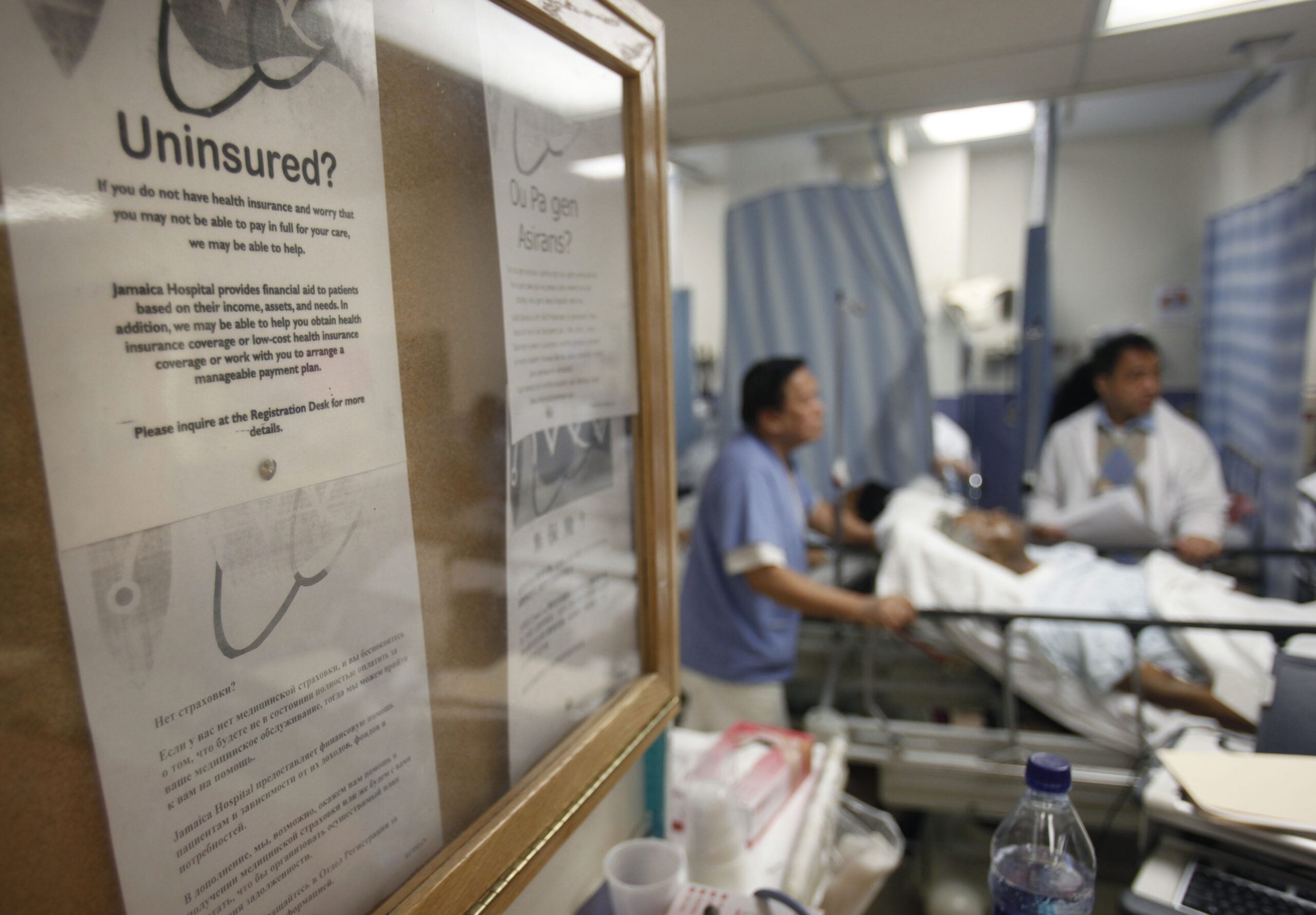
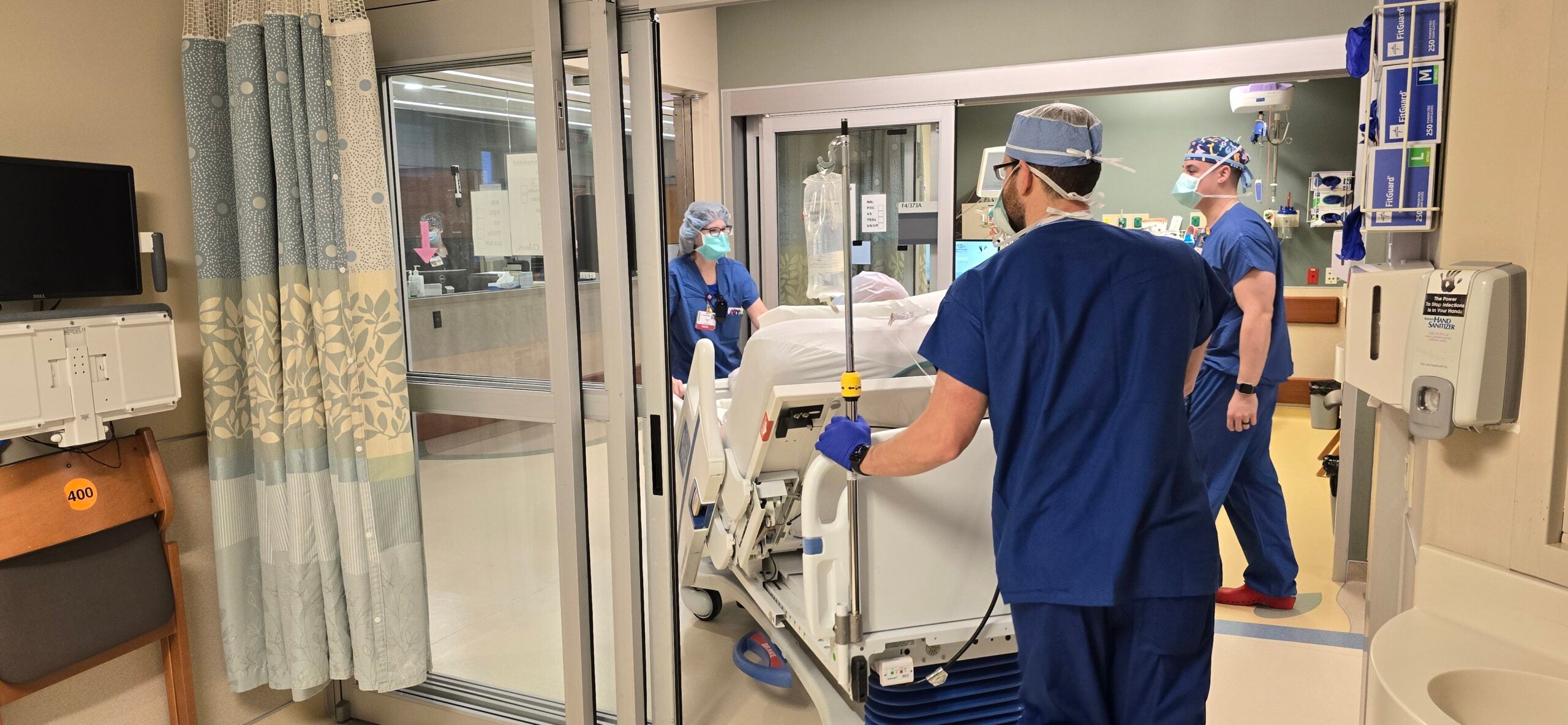
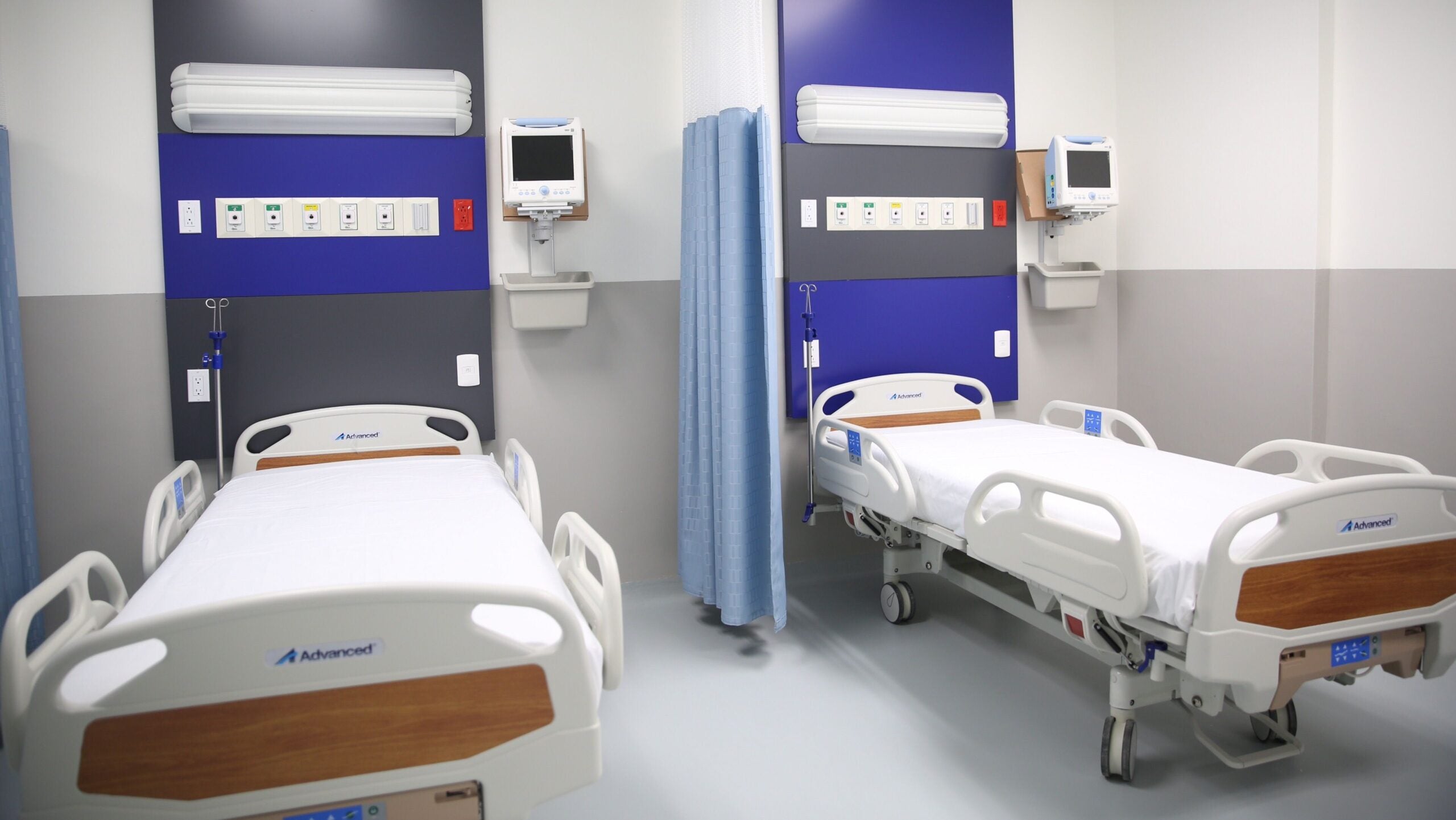
Some rural hospitals across Wisconsin are having a difficult time finding beds for COVID-19 patients and those with other illnesses. Some people are being transferred hundreds of miles away because closer facilities in urban areas are full.
The difficulty of finding a place to refer patients was frequently mentioned by members of the Rural Wisconsin Health Cooperative in a monthly meeting last Friday, according to Executive Director Tim Size. The cooperative represents 43 rural hospitals across the state.
“What I’ve heard are people having to call five to 10 hospitals to transfer someone to a higher level of care,” said Size. “I have not yet heard of someone who could absolutely not be transferred, but we’re very close to that.”
News with a little more humanity
WPR’s “Wisconsin Today” newsletter keeps you connected to the state you love without feeling overwhelmed. No paywall. No agenda. No corporate filter.
Size said the surge in COVID-19 cases has overwhelmed hospitals across the state, leaving many at or near capacity.
There were 7,777 new cases of COVID-19 reported by the Wisconsin Department of Health Services on Friday, the state’s fourth record-breaking day for new cases in the past week. The state reached another dark milestone this week when its seven-day average for new cases exceeded New York’s highest seven-day average from April.
Dr. Ben Turner with Essentia Health in Hayward said they’re caring for patients with more significant needs than they’re used to providing.
“Generally, a lot of these people we would send out of here to a tertiary center,” said Turner. “With the centers being full and not having access, we’re keeping a lot of these patients that we normally wouldn’t. So, it’s not only more challenging for us, but it’s more challenging for the staff.”
Mayo Clinic Health System announced earlier this week that its hospitals in northwestern Wisconsin were full to capacity, including facilities in Barron, Bloomer and Eau Claire.
Turner is among physicians who serve on the medical executive committee for Hayward Area Memorial Hospital, which has been operating at around 75 percent of its capacity. Fellow physician Dr. Devon Dannen, chief of medicine at Northlakes Community Clinic, said they’ve sent people as far away as Eau Claire and La Crosse to receive care.
“But you have to remember that COVID is very high in all the (counties) in our region right now,” said Dannen. “So, it is not a matter of like, just find a bed in a farther-away hospital. Those hospitals are also full, and hospitals are having to triage and (are) saying they won’t see patients that haven’t been seen in their system in the last six months because they have so many patients.”
Dannen said it’s a problem that’s affecting the entire hospital system. In Ashland, Dr. Jill Schenk, physician and medical staff president of Memorial Medical Center, said they’re not at capacity. But the hospital has seen a higher volume of patients. Schenk said they’re also seeing slower transfers of ICU patients than normal.
“We are working with a lot of regional partners to find beds and space and resources,” said Schenk. “For those patients, we have been able to get folks to where they need to go in those situations.”
The Ashland hospital typically sends patients to facilities in Duluth, but it’s recently sent patients to the Twin Cities for care if Duluth has been unable to accept patients or provide the services required. Great Divide Ambulance Service, which serves Ashland and Bayfield counties, recently had around 30 requests to transport patients from northern Wisconsin to far off destinations, including Eau Claire, La Crosse and Rochester, Minnesota.
“Regional specialty centers, which are in our location in Duluth, have been on diversion because they’ve been unable to take patients,” said Rob Puls with Great Divide Ambulance Service.
Puls said Duluth hospitals have opened up more in the last several days. Dr. Nick Van Deelen, chief medical officer with St. Luke’s Hospital in Duluth, said in a press conference on Thursday that they’re shifting resources to handle more patients.
“Those changes include adjusting staffing, dedicating an entire unit of 40 beds for patients with COVID-19 and adding 24 additional critical and ICU beds to our already existing 25 to help provide care for those most critically affected by this disease,” said Dr. Van Deelen.
Dr. Jon Pryor with Essentia Health in Duluth said they’ve also transferred patients to other hospitals within their system to make room for patients with more severe illnesses.
“We’ve taken patients from Michigan and Wisconsin. We’re trying to do a little bit less of that, if possible, so we can have our ICU beds available for the Twin Cities when they’re full,” said Dr. Pryor.
While hospital systems are stressed, health officials are urging people not to put off care even as some hospitals are postponing elective surgeries.
Size said hospitals across the region are reaching a point where they may not be able to provide care for all those in need.
“They can only do so much. They can only handle so many patients,” said Size. “We’re just about at the cap of what our rural hospitals and urban hospitals can handle.”
Wisconsin Public Radio, © Copyright 2026, Board of Regents of the University of Wisconsin System and Wisconsin Educational Communications Board.