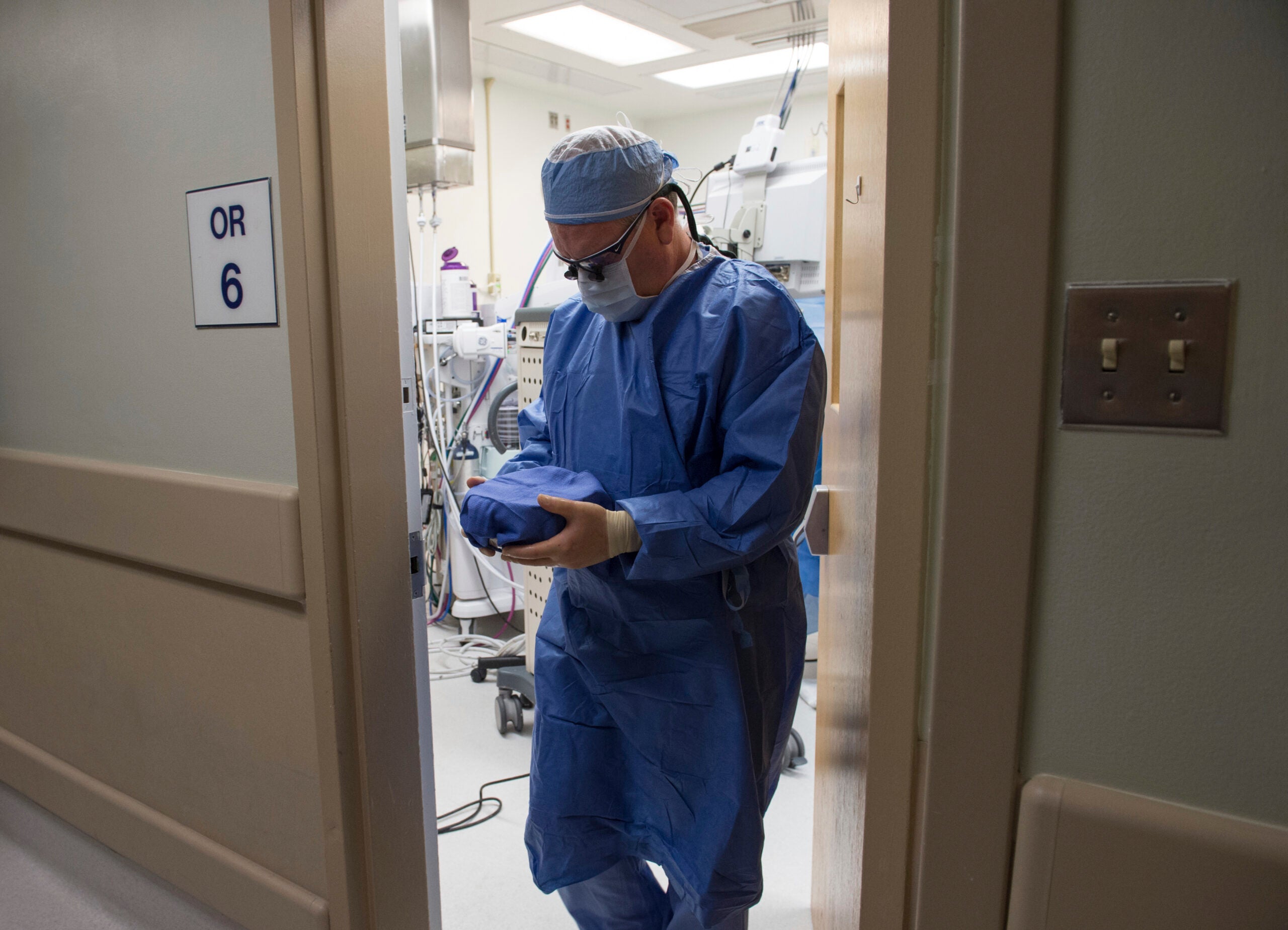
Last year, a record 39,700 organ transplants were performed in the United States. But this year, lifesaving transplants have been dramatically affected as the coronavirus pandemic has caused a shortage of ICU beds, fewer donations and severe COVID-19 complications with new organ recipients.
In the spring, Dr. Nikole Neidlinger, associate director of the University of Wisconsin Organ and Tissue Donation program, said that by late March, the number of transplants had dropped by half compared to the first two months of the year in Wisconsin. Nationwide, this statistic is similar.
Much of that reduction comes from a steep decline in the number of kidney transplants, though a substantial drop in heart, lung and liver transplants was also recorded.
News with a little more humanity
WPR’s “Wisconsin Today” newsletter keeps you connected to the state you love without feeling overwhelmed. No paywall. No agenda. No corporate filter.
The impact on kidney transplants stems from a variety of factors, but most notably it has to do with the somewhat elective nature of living kidney donations, said Dr. Didier Mandelbrot, medical director of the UW Health Kidney and Pancreas Transplantation Program.
“While many organ donations would be from deceased donors to recipients who might be at death’s door … in most cases (living kidney donation) can quite readily be rescheduled for one month, or two or three later,” Mandelbrot said.
In April, living kidney transplants were put on hold because people with end-stage kidney disease are typically on dialysis and there’s more flexibility with the procedure date, he said.
“Transplant is better,” he said. “It prolongs life, it improves the quality of life, but dialysis treatments can sustain life. In most cases, the transplant can be delayed somewhat, though there are exceptions to that,” Mandelbrot said.
The U.S. already suffers from a shortage of transplantable organs. Nearly 114,000 people are on the national waiting list for a lifesaving organ transplant.
In recent months, deceased donor transplants from deceased organ donors numbers have worked their way back up to pre-pandemic levels, Neidlinger said. But, she suspects the number of donated organs has dropped because of the pandemic — and people’s hesitance to go to the emergency room early in the pandemic.
“There are probably organs that have been lost in patients who are at home and are suffering, don’t have coronavirus, but are suffering from heart attacks or having strokes or other injuries,” she said. “There have been instances where people have died at home and been excluded from the possibility to donate.”
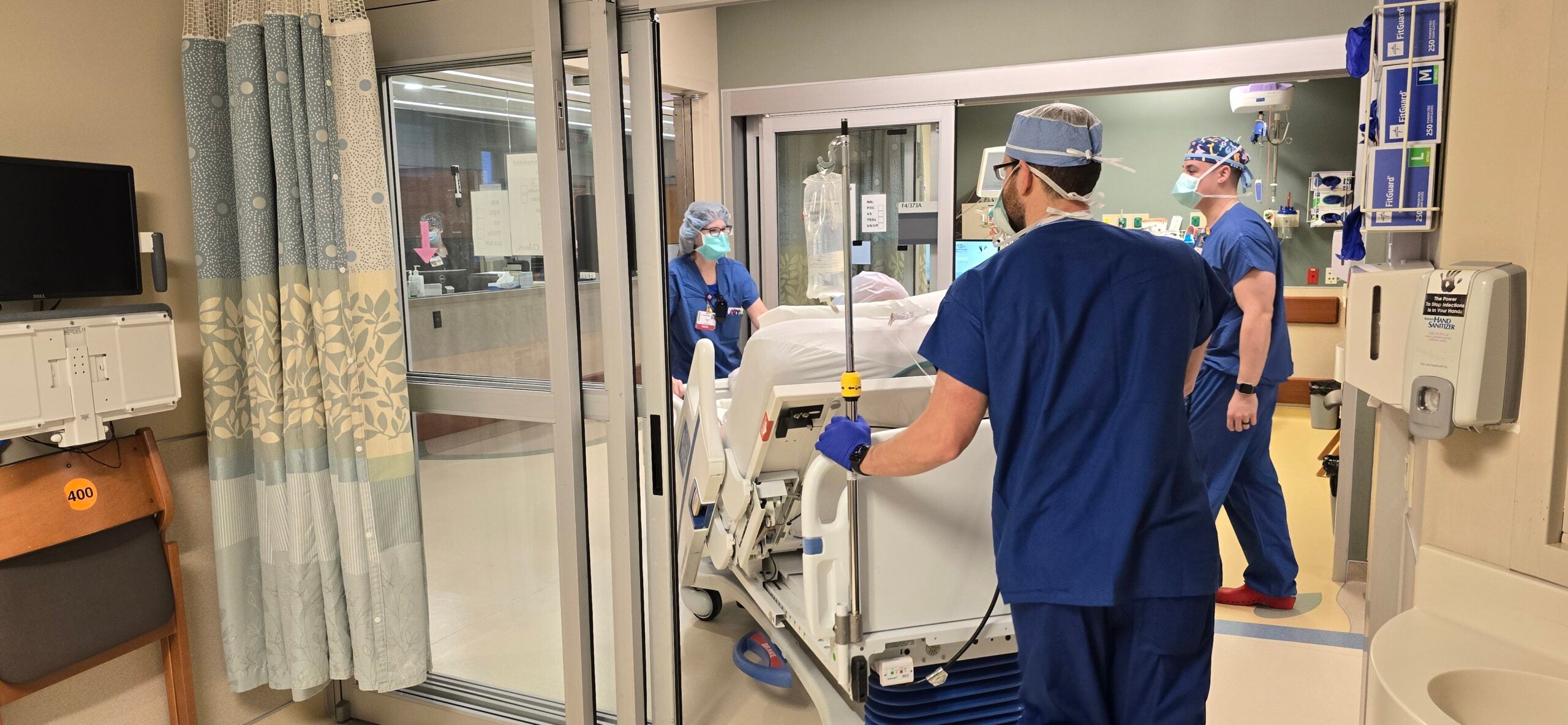
Transplants have also struggled because of ICU bed shortages, Neidlinger said.
“Patients who may be potential organ donors after having died from something like a stroke, an anoxic injury or a car crash, they need an ICU bed and ICU resources while we work with the organs and do the testing needed for recipients,” she said. “In the current climate where ICU beds are really challenging to come by, we’ve really been struggling.”
For patients who do receive a transplant, they are at higher risk of both getting infected and facing severe complications from COVID-19 because end-stage organ disease and immunosuppression after a transplant weaken the body’s immune response.
Organs from people who have died of COVID-19 are not being accepted because of a lack of certainty over how the disease affects various organs in the body.
“However, there’s a lot of questions about that,” Neidlinger said. “Because in the past … we’ve been able to navigate, for instance, transplanting organs from people who’ve died of other respiratory viruses, like H1N1, influenza.”
Wisconsin Public Radio, © Copyright 2026, Board of Regents of the University of Wisconsin System and Wisconsin Educational Communications Board.