Wisconsin is among 23 states considered coronavirus “hot spots” which saw an increase in COVID-19 cases at nursing homes and assisted living facilities as the virus continued to spread throughout communities in late June and early July, according to a Kaiser Family Foundation review of state data.
But Wisconsin did not reach the levels seen in some states, like Texas and Florida, which had increases of 47 and 51 percent respectively, in long-term care coronavirus cases over a two-week period ending July 10. Wisconsin had a 5-percent rise in COVID-19 cases at long-term care facilities, while cases statewide surged 32 percent.
“I think it validates the hard work that is going on in Wisconsin,” said John Sauer, president of LeadingAge Wisconsin, an association of long-term care organizations. “Even though the state saw an overall increase in the number of COVID-19 cases, in the long-term care world, we haven’t seen that dramatic kind of spike.”
News with a little more humanity
WPR’s “Wisconsin Today” newsletter keeps you connected to the state you love without feeling overwhelmed. No paywall. No agenda. No corporate filter.
Between June 24 and July 9, Wisconsin set two new daily records for the number of coronavirus cases and Gov. Tony Evers urged people not to travel for the Fourth of July holiday to try to slow spread of the virus.
Many communities, especially college towns, were experiencing a rapid increase in infections among young people at the time which was helping drive numbers upward. In response, Dane County issued a new public health order closing indoor bar service and reducing restaurant capacity to 25 percent.
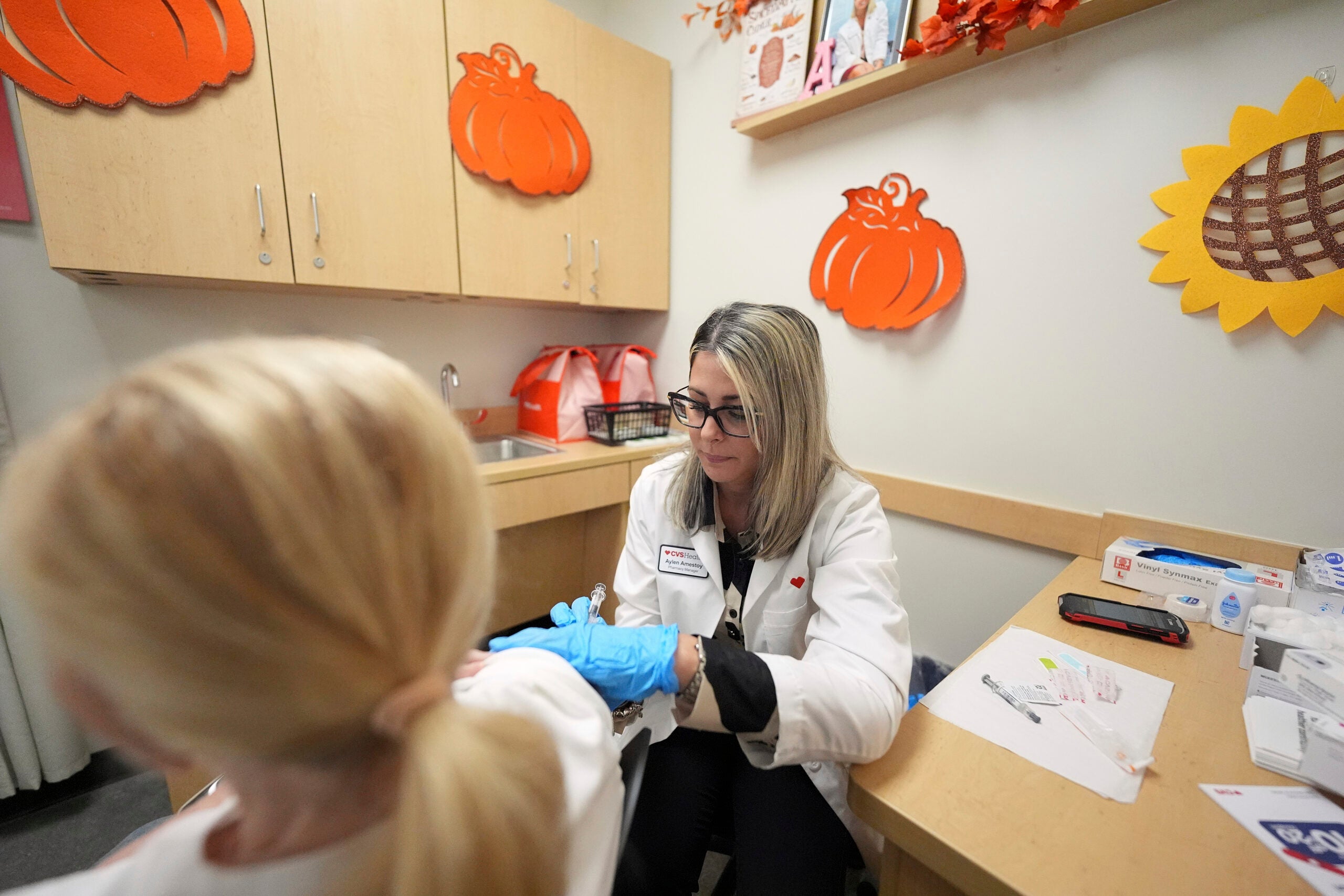
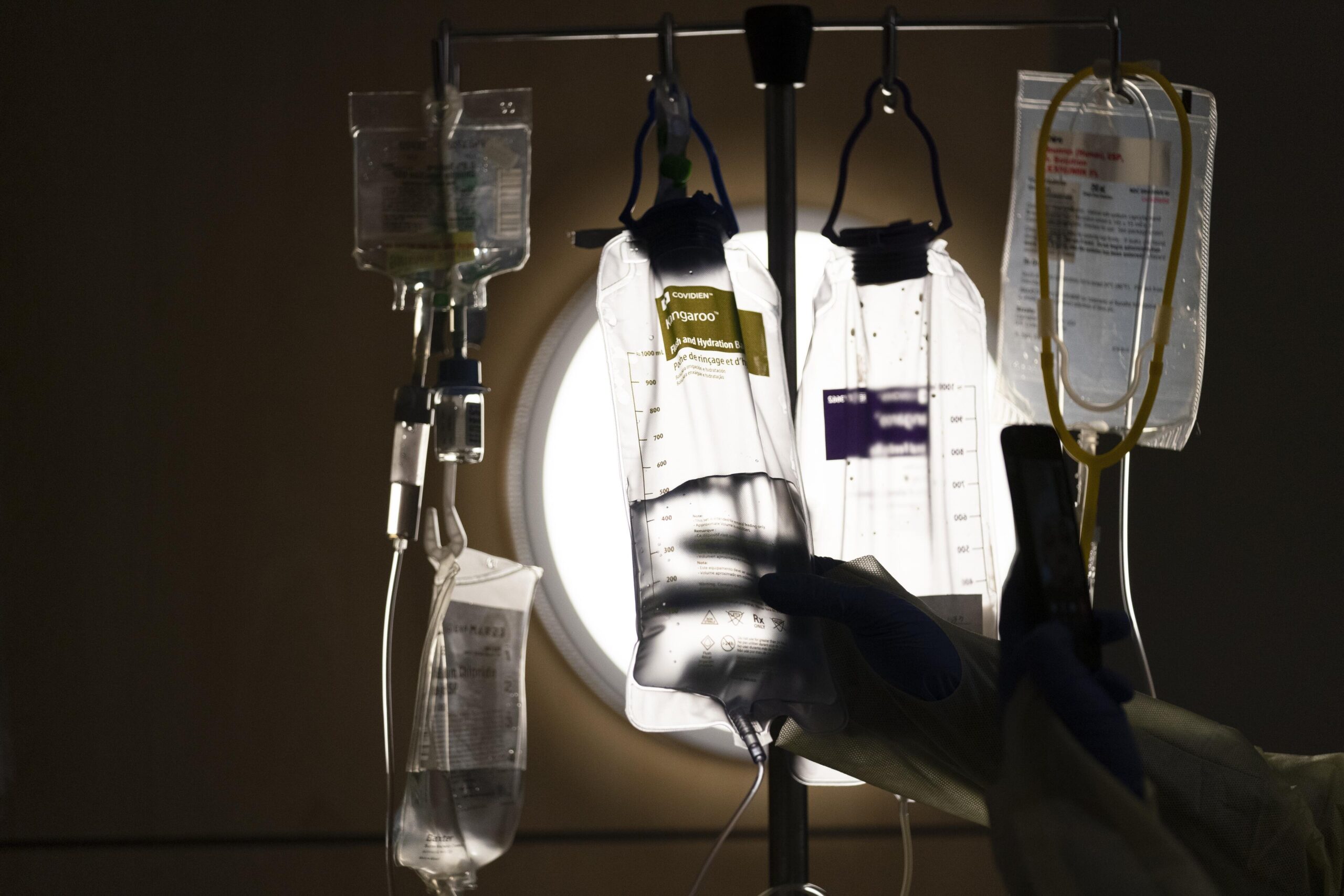
Nursing homes and assisted living facilities have strict measures in place to prevent the coronavirus from getting in or spreading inside facilities. Visitation was temporarily banned and infected patients were isolated. Regardless of these precautions, the Kaiser review shows facilities continue to see the number of cases go up, and it can have deadly consequences. The elderly are more vulnerable to severe illness and death from the disease compared to younger people. According to state data, at least 41 percent of all Wisconsin’s COVID-19 deaths have been in long-term care facilities.
As of July 15, Wisconsin had 231 active investigations at nursing homes and assisted living facilities. A single positive case of coronavirus triggers an investigation. State health officials say detecting COVID-19 in a nursing home is an indicator that the nursing home is following proper notification procedures and working to protect their residents and employees by using appropriate isolation and infection control practices.
But advocates for the elderly say more needs to be done including regular, ongoing testing and providing adequate personal protective equipment.
“Unfortunately, the virus continues to spread like wildfire through nursing homes, both in Wisconsin and across the country. Basic precautions to protect residents and staff are still not in place,” said Lisa Lamkins, federal issues advocacy director for AARP Wisconsin. “Congress has passed four bills to address the devastating impact of coronavirus, yet they’ve barely touched on the crisis in long-term care facilities.”
In May, Evers directed $100 million in federal pandemic funding from the CARES Act to nursing homes and emergency medical services, and also announced a plan to test all nursing home residents and workers.
But the lag in getting results sometimes means the disease can spread before a patient or staff member knows they’re infected. Sauer said a rapid, reliable test needs to be used in accordance with best infection control practices.
“If the state and federal governments could work together to see how the provider community could have access to rapid results testing, that would do a lot to further protect those under our care,” he said.
Even before the pandemic, nursing homes were struggling financially and experiencing staff shortages. In Wisconsin, more than 30 skilled nursing homes have closed since 2016.
Wisconsin Public Radio, © Copyright 2026, Board of Regents of the University of Wisconsin System and Wisconsin Educational Communications Board.