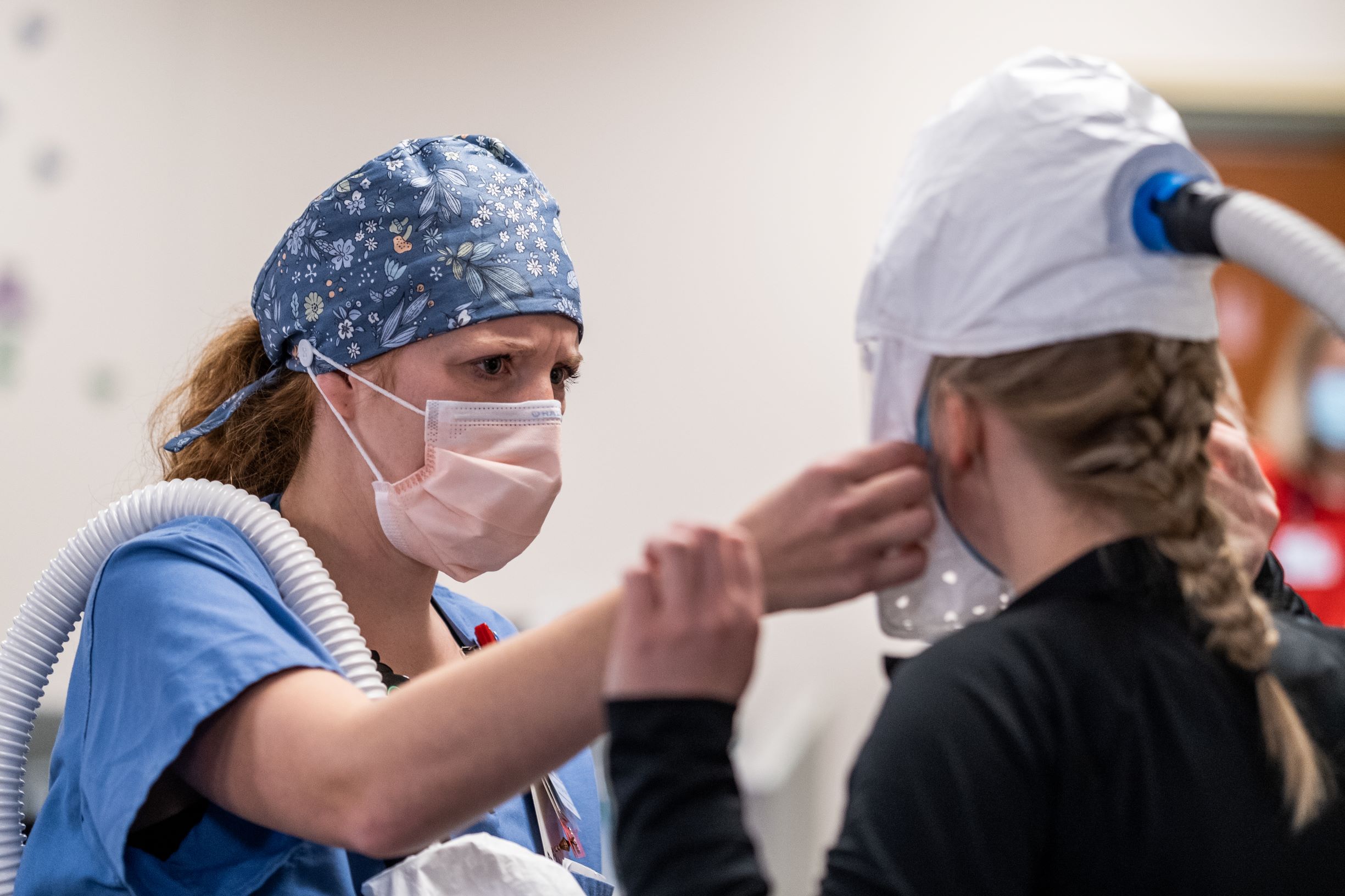
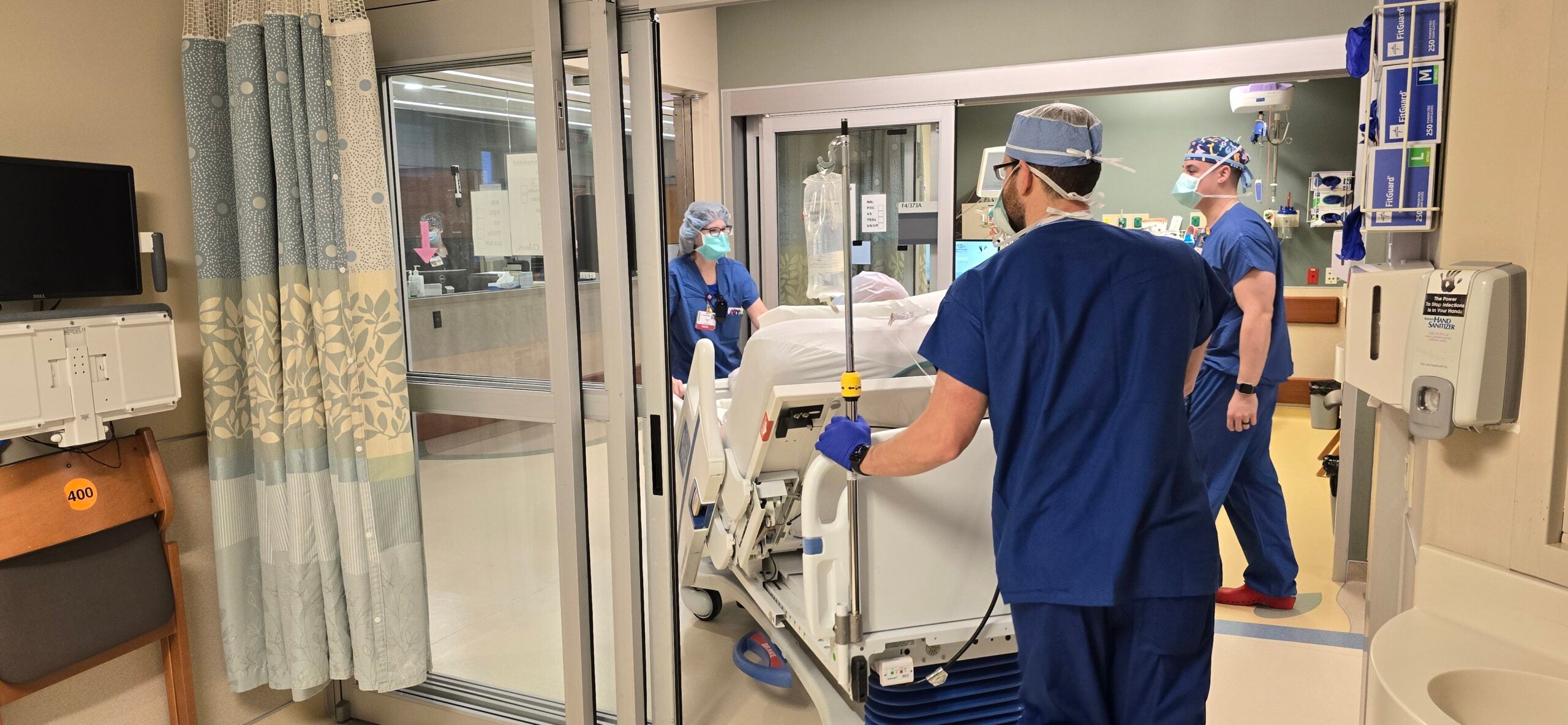
Hospitals in Wisconsin are taking extraordinary measures in the midst of a surge of severe COVID-19 cases.
In Wausau and Merrill, Gov. Tony Evers’ administration is calling on retired and volunteer nurses and health care workers to help staff two nursing homes that will care for some patients in recovery from COVID-19, freeing up hospital beds for acute cases.
In Green Bay, the Federal Emergency Management Agency announced late Monday that it would send a team of 20 U.S. Navy medical providers to support staff at Bellin Hospital.
News with a little more humanity
WPR’s “Wisconsin Today” newsletter keeps you connected to the state you love without feeling overwhelmed. No paywall. No agenda. No corporate filter.
The Wausau initiative, the first of its kind in the state, will allow Aspirus and Marshfield Clinic health systems to discharge patients to two nursing homes operated by North Central Health Care. Those nursing homes, Mount View Care Center in Wausau and Pine Crest Nursing Home in Merrill, will admit up to four COVID-19 patients per day who are past the point of being contagious but aren’t yet well enough to go home.
“There was a request from the health systems in our area for any assistance for relief,” said Jarret Nickel, North Central Health Care’s COO.
The pressures on hospitals from the latest surge in cases, nearly two years into the pandemic, has been intense. In the north-central region, which includes Wausau and much of the Northwoods, there were 192 patients hospitalized with COVID-19 on Tuesday, according to Wisconsin Hospital Association data — not far from the peak of 255 patients who were hospitalized in the region in the fall of 2020, during the worst spike in infections in Wisconsin and before vaccines were widely available.
Hospitals have struggled with staffing as the number of patients has swelled, and nursing homes across the state have faced staffing crises of their own. Nickel said staffing at North Central’s nursing homes has been relatively stable. But the organization will rely on a state medical reserve corps to provide staff for the additional beds they’re making available.
The state program is called the Wisconsin Emergency Assistance Volunteer Registry, or WEAVR. Anyone can volunteer, but the program is designed for licensed health workers, including those who have recently retired or who are still in training.
Nickel said the scale of the emergency program will depend on the number of short-term health care staff North Central can get through the WEAVR program. If North Central finds enough workers, it might open up additional units to accommodate as many as 20 more COVID-19 patients, Nickel said. He expects the emergency period to last for eight to 10 weeks.
‘Our hospitals are at the breaking point’
As of Tuesday, there were 1,653 patients in Wisconsin hospitalized with COVID-19, 418 of whom were in intensive care units, according to the Wisconsin Hospital Association. Those numbers were down slightly from peaks this month of 1,714 and 443, respectively, but the declines were slight and not sustained.
In a statement, Aspirus Wausau Hospital Emergency Department Director Robin Rudie said Aspirus was one of the many health systems in Wisconsin delaying non-emergency surgeries and other procedures that require a hospital stay.
“When you need access to emergency care or care that requires an inpatient hospital bed, that care may be delayed or it might be harder to come by,” Rudie said.
Aspirus has also begun to transfer some patients to other hospitals within its system, according to where there are open beds.

New COVID-19 infections in Wisconsin have been generally rising since early November, with brief periods of decline. But with the holidays leading to more gatherings and the presence of the new, more transmissible omicron variant of the disease present in Wisconsin, experts expect a new surge from already high infections and hospitalizations.
“Our hospitals are at the breaking point,” said Dr. Ben Weston, Milwaukee County’s chief health policy adviser. “And with omicron making up a substantial portion of new cases — likely the majority, as we see updated sequencing — we have a flood of cases coming.”
According to state data, people who are fully vaccinated are 11 times less likely than the unvaccinated to be hospitalized and 12.5 times less likely to die from the disease.
One question scientists are studying is whether omicron tends to cause less severe infections. Some data suggest that could be the case, but on Monday, the World Health Organization said it was too early to reach that conclusion.
In Wisconsin, a less severe variant that spreads more quickly could still worsen the crisis in hospitals if even a fraction of those who become infected end up with severe disease. On Monday, Wisconsin health officials in a statewide health advisory and press conference urged people to get vaccinated and boosted, to keep holiday gatherings small and to get tested for COVID-19 before gathering.
FEMA to send a team of medical workers to Green Bay
Twenty medical workers from the U.S. Navy, including doctors, nurses and respiratory therapists, will support work at Bellin Hospital in Green Bay, the military announced. The federal effort has already sent teams to five states, but this is the first such deployment to Wisconsin. It also announced a similar deployment to Indiana.
At a press event for Milwaukee County on Tuesday, Dr. Chad Craig, chief medical officer of Ascension Wisconsin, said he hopes it is not the last deployment of federal resources to help in the fight against COVID-19 here.
“All hospitals throughout Milwaukee are short-staffed, and are experiencing the stresses of surging (COVID-19 cases),” Craig said. “Our organization is part of statewide planning and has been in communication with DHS … regarding potential federal resources that have been requested by the state. We certainly welcome any support that we can get.”
Wisconsin Public Radio, © Copyright 2026, Board of Regents of the University of Wisconsin System and Wisconsin Educational Communications Board.