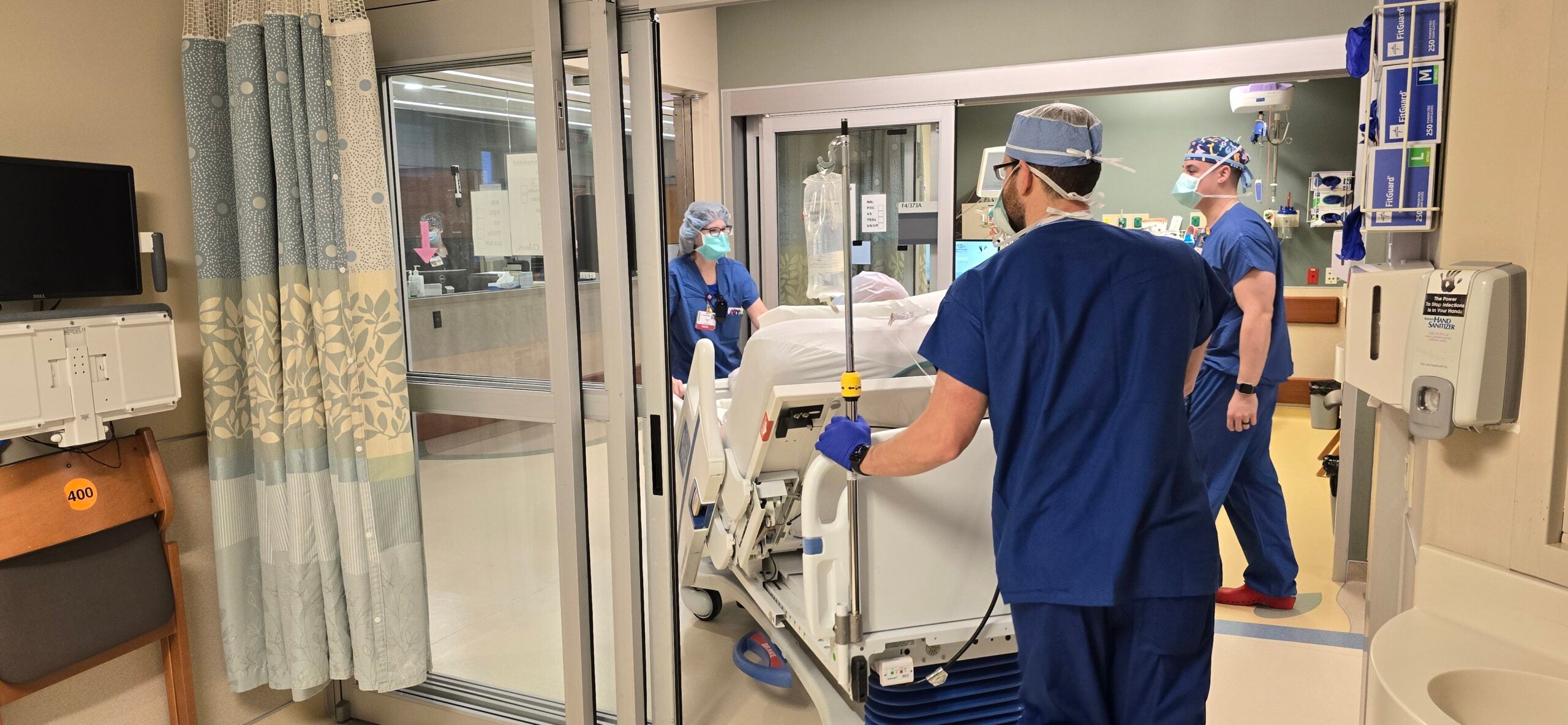
Wisconsin has seen four major hospital mergers either finalized or announced over the last year, and some experts fear that increased health care consolidation could lead to higher prices for patients.
Late last year, Gundersen Health System and Bellin Health completed a merger. As did Advocate Aurora Health and Atrium Health. That October, Marshfield Clinic Health System and Essentia Health announced they were in talks to merge. And last month, Froedtert Health and ThedaCare also announced plans to merge.
Hospital officials say the mergers are meant to improve patient care and stem from organizations having similar missions and visions.
News with a little more humanity
WPR’s “Wisconsin Today” newsletter keeps you connected to the state you love without feeling overwhelmed. No paywall. No agenda. No corporate filter.
Health care mergers are nothing new. The industry has consolidated substantially over the last two decades, and at a more rapid pace since 2010, according to a 2020 study by Harvard Medical School scientists.
Ashley Swanson, associate professor of economics at the University of Wisconsin-Madison, said hospital mergers — on average — increase prices, while having a negligible effect on patient care.
Swanson said those price increases impact insurers in the short-term, but lead to higher insurance premiums and higher out-of-pocket costs for patients in the long-term.
“It seems like they primarily increase prices when the merging hospitals are located close to one another,” she said. “But there is some relatively new evidence suggesting that cross-market mergers can sometimes increase prices as well.”
Cross-market mergers are consolidations of entities that cover different geographic areas. Those have been the primary health care mergers in Wisconsin recently. For example, Froedtert serves the southeastern part of the state while ThedaCare primarily serves northeast and central Wisconsin.
Swanson said more research is needed to evaluate the full effect of cross-market mergers on prices, and it’s too early to know what the effects of recent mergers will be in Wisconsin.
“Putting those two things together — higher prices and no better care — it doesn’t seem like mergers are a good deal for patients, payers or society,” she said. “That’s all on average, so that may be averaging out beneficial effects of some mergers against detrimental effects of other mergers.”
Brian Potter, chief financial officer for the Wisconsin Hospital Association, said health care mergers in Wisconsin haven’t been aimed at eliminating competition. Rather, he said they’ve been mergers to build capabilities and scale.
“These different systems bring different strengths and different weaknesses,” he said. “I think that’s what’s driving a lot of these mergers as the health care environment gets more challenging, financially, workforce-wise and regulatory-wise.”
Potter said examinations of mergers’ effects on prices often look at costs for patients with commercial insurance, which he believes doesn’t account for low reimbursement rates hospitals receive from programs like Medicare and Medicaid.
On average, Potter said Medicare and Medicaid patients make up about 60 percent of a Wisconsin hospital’s business. While mergers may affect prices for commercial insurers, he said funding formulas for government insurance programs remain the same.
“Medicare and Medicaid both underpay the cost of care,” he said. “The only way you can survive with that much of your business is to get more efficient.”
Despite recent mergers, Potter said he thinks there’s still a lot of competition between health care providers in the state.
“We (put) a 30-mile radius around every town, and — in almost every case — there’s at least two competing hospitals,” he said. “It’s a very competitive state on both the provider and on the payer side, which is what you don’t typically see when there’s a lot of mergers.”
Zachary Levinson is a project director for the nonprofit health policy organization KFF, and examines how health care business practices impact costs and affordability. Even when hospitals merge across markets, he said there’s some research to suggest it causes prices to increase because it can improve health care providers’ bargaining position with insurers.
“There might be a case where a health system includes a must-have hospital in a given region,” he said. “It’s negotiating with a health plan that operates in multiple regions, and it uses its leverage as a key must-have institution in a given region to essentially receive high prices across the markets in which it operates.”
Wisconsin Public Radio, © Copyright 2026, Board of Regents of the University of Wisconsin System and Wisconsin Educational Communications Board.