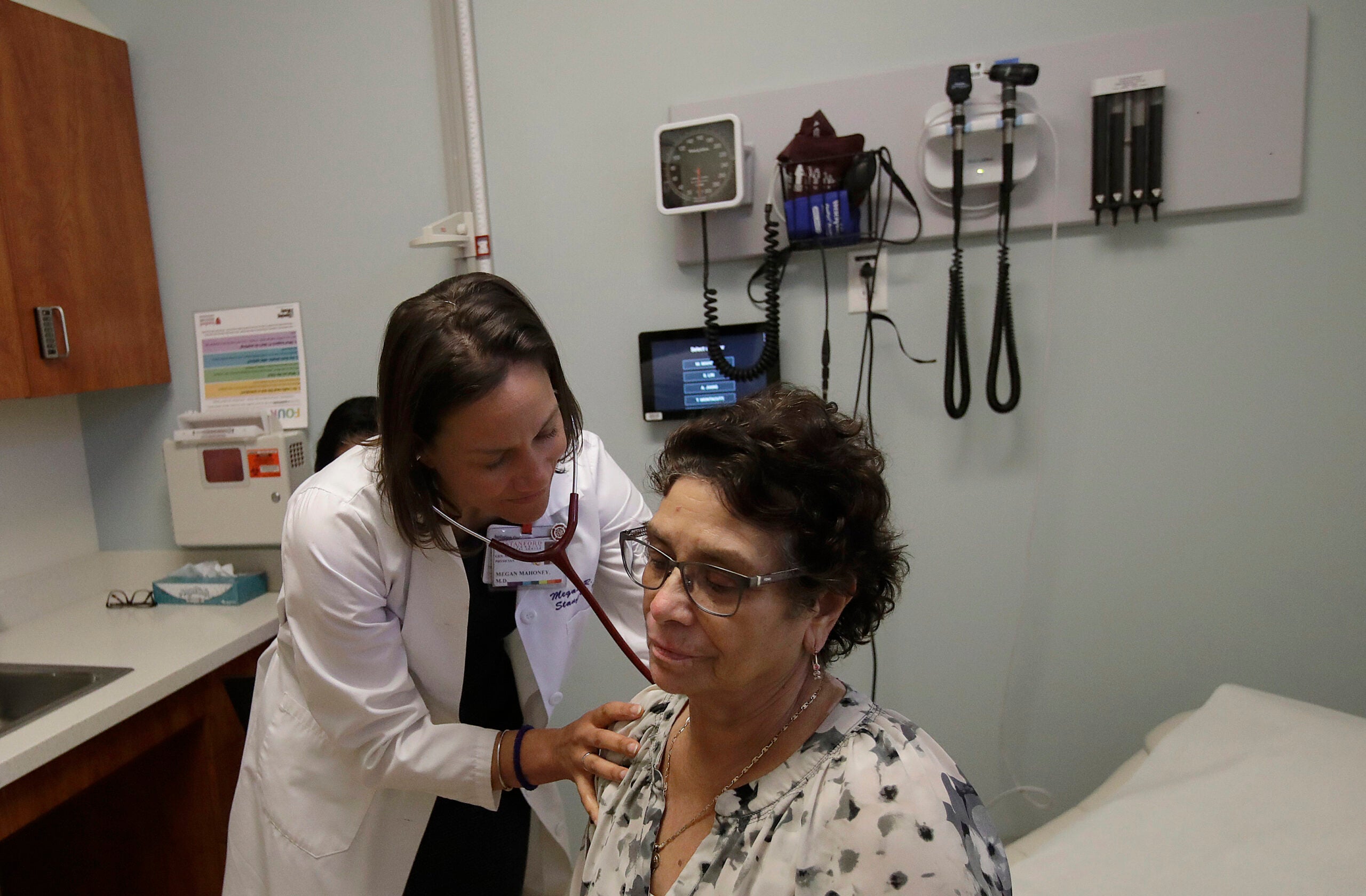When Froedtert Health and ThedaCare announced an agreement in September to merge operations, the news marked the fourth time in a year that major Wisconsin health care providers had disclosed or finalized plans to combine forces.
The news also underscored the growth of consolidation in health care nationally. Almost 1,900 hospital mergers happened from 1998 to 2021, according to American Hospital Association reports. This year, the pace of mergers appears to be speeding up from last year, according to the health care consultant Kaufman Hall.
At the University of Pennsylvania, Dr. Rachel Werner studies the impacts of hospital mergers and testified in October at a Pennsylvania statehouse hearing to warn about the effects of widespread consolidation.
News with a little more humanity
WPR’s “Wisconsin Today” newsletter keeps you connected to the state you love without feeling overwhelmed. No paywall. No agenda. No corporate filter.
“It is important to recognize that the burden of these higher prices ultimately falls on patients through higher health care insurance premiums,” Werner said at the hearing. “By and large, (evidence) suggests that the quality of care is worse in highly consolidated markets compared to markets with more competition.”
Werner, who also leads the Leonard Davis Institute of Health Economics, recently joined WPR’s “The Morning Show” to discuss why more hospitals are merging and why consolidation can lead to increased health care costs.
The following was edited for clarity and brevity.
Kate Archer Kent: What main factors are driving hospital consolidations?
Dr. Rachel Werner: Health care consolidation is certainly not just happening in Wisconsin. It’s a trend we’re seeing across the entire country, and it’s impacting every aspect of health care from hospitals to physician practices for hospitals.
Merging has several potential benefits. Hospitals often claim that it allows them to increase the coordination of care across hospitals. It reduces duplication of services within a market. It can actually improve integration and management and also reduce operating costs for a hospital. So, hospitals look at mergers as a way to improve their efficiency and potentially increase access to acute care services.
Mergers in general, whether it’s a for-profit hospital or not-for-profit hospitals, have a detrimental effect on prices. They tend to increase the price that insurers pay for care for commercially insured individuals. And they don’t really have any improvement in quality. Really, what we see are just higher prices — no improvement for patients.
KAK: You called hospital mergers “a trend.” When did you start seeing this practice?
RW: It’s not a new trend or a new challenge. It has rapidly accelerated recently.
Between 1998 and now, we’ve seen the number of hospitals going from about 8,000 down to just over 6,000 hospitals. That’s really a 25 percent decline in the number of hospitals in this country, in part due to mergers. And at the same time, the number of hospitals that are part of a larger system has increased… By 2017, about two-thirds of all hospitals were part of a larger system as compared to about half in 2005.
It’s not clear why it’s going on. The Affordable Care Act may have accelerated this trend and increased hospitals feeling that they need to merge to be able to respond to some of the incentives in the Affordable Care Act. But it’s certainly been a long-term trend that we’ve been watching in health care.
KAK: You testified before the Pennsylvania House of Representatives on hospital consolidation. You told lawmakers that mergers can increase commercial health care prices by up to 50 percent. Why can mergers increase costs to this degree?
RW: What happens is that hospitals negotiate with insurers over network and over price, and insurers want to build a network of hospitals that’s a good value to their consumers and their customers. When there are two hospitals that are in the same market and they are perceived to be of equal value… those hospitals have to compete to be included… The insurer can then bargain on price. … But when two hospitals merge, the insurer will want to include the merged hospital in the network, but there are no other good substitute options in that market… This results in higher prices.
KAK: You’ve warned about the effects of private equity investment in health care. How are investors affecting health care consolidation?
RW: Acquisition of hospitals by private equity firms has soared over the past decade. This has really sparked a debate about the growing influence of private equity in health care and how it might affect all the same things we’re concerned about with consolidation, which include costs, quality and access.
Private equity firms, at least in the physician market, tend to acquire relatively small physician practices one at a time. And the Federal Trade Commission doesn’t oversee or monitor those kinds of acquisitions that are less than $100 million. So, while a private equity firm may be acquiring just one small hospital or one small practice, over time within a market they do more and more of those small deals and it results in market consolidation.
At the end of the day, that market consolidation is no different than the market consolidation that we see from hospital mergers that we’ve been talking about. And this increase in consolidation can lead to higher commercial prices with no positive effects on quality. It may also decrease access to care for patients.
READ MORE: Froedtert, ThedaCare plan to merge, hope to launch combined health system by end of 2023
READ MORE: Wisconsin sees 2 major hospital mergers finalized back to back
KAK: How could state lawmakers address problems or begin to address problems stemming from hospital consolidation?
RW: States should continue to actively monitor mergers and try to require hospitals to be more transparent and have waiting periods around mergers. States should also more actively monitor the contracting practices of insurers to prevent anticompetitive behavior on the part of those contracting practices. States can also encourage more transparency related to price and quality, which allows consumers to try and choose a hospital that’s best suited for their needs. And that really promotes competition, to counter some of the negative effects of consolidation in the market.
Wisconsin Public Radio, © Copyright 2026, Board of Regents of the University of Wisconsin System and Wisconsin Educational Communications Board.