Access to maternal health care is disappearing in rural America. We find what is causing the shortage, and how to reverse it. While job loss can have a financial impact, it turns out that the emotional toll on our sense of self can be even more significant. We find out why, and how to mitigate the effects. We also talk about the results of a federal inquiry into the Wisconsin Veterans Home at King, which showed the facility didn’t meet three of 158 standards required of state veterans nursing homes.
Featured in this Show
-
Federal Inspection Of The Wisconsin Veterans Home At King Finds Three Federal Standards Not Met
On Monday the U.S. Department of Veterans Affairs released the results of a federal survey of the Wisconsin Veterans Home at King, requested by U.S. Senator Tammy Baldwin in January. The report showed the home didn’t meet three of 158 standards required of state veterans nursing homes. We talk to a reporter covering the allegations against King about this news.
-
As Rural Hospitals Make Cuts, Maternal Health Care Is Often First To Go
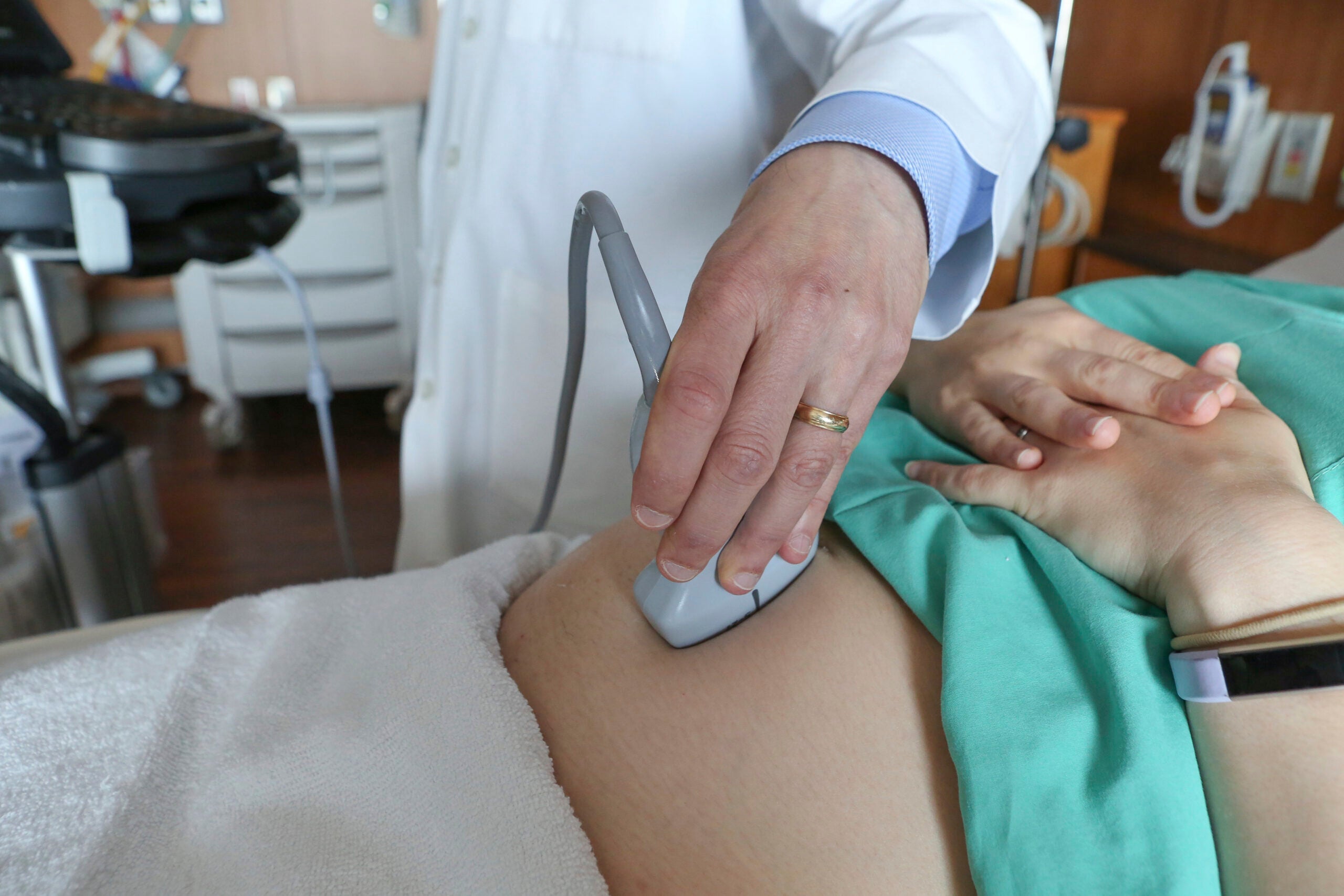
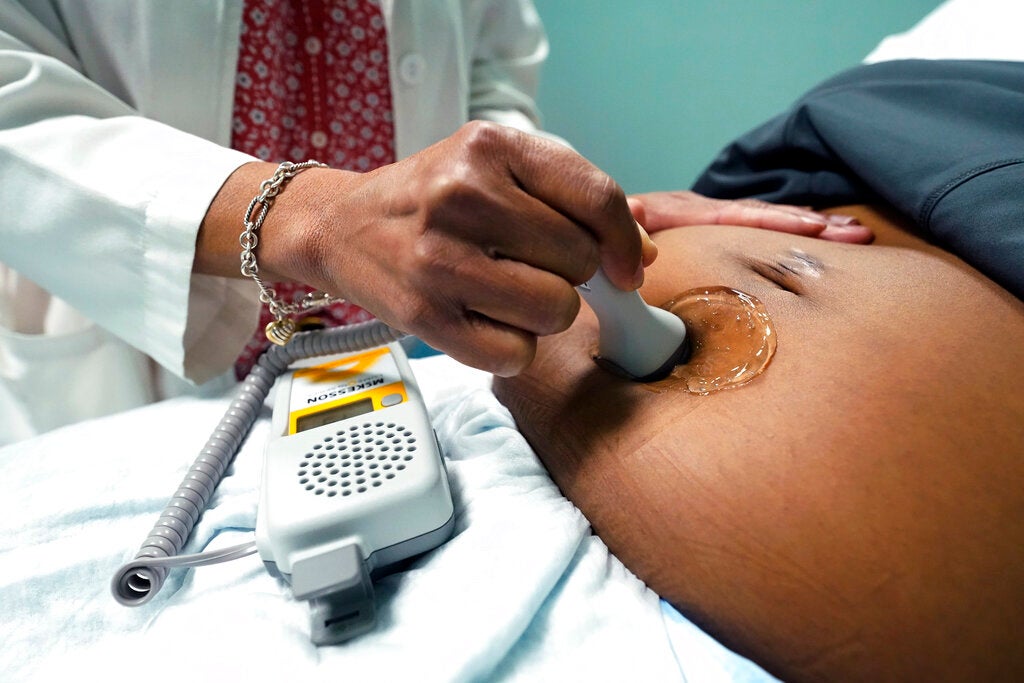
Some women take it for granted that when it’s time to give birth, they can go to a nearby hospital. For women in the most rural parts of the United States, it’s not so simple.
As rural hospitals and clinics are making budget cuts, maternal health care services are often the first to be eliminated, said Dina Fine Maron, health and medicine editor at Scientific American.
“Only about 6 percent of the nation’s OB-GYN’s work in rural areas; so as a result, some women I spoke to for this article told me rather harrowing tales of how women in their area have to drive great distances to deliver a baby or even in some cases to get pre-natal care,” Maron said.
Less than half of rural women live within a half-hour drive of the nearest hospital offering obstetrical services, and about 88 percent of women in rural towns live within an hour’s drive. Maron said that means some women end up camping out near the hospital around their due dates, with a family member or in a hotel. Delivering in the back of a car or in the emergency room on the way to the hospital is how some rural women give birth.
Because of these distance issues, some women may not be getting as much prenatal care as they should. Maron said family physicians offer obstetric services in some areas, but that’s not always enough, especially for a complicated pregnancy.
“The reality is if it looks like a woman might have a complicated pregnancy or need certain kinds of prenatal testing or gene counseling, a family physician would not be well-poised to offer all of those services,” she said.
The problems affecting maternal services are part of the larger trend of what’s happening in rural health care.
People who live in rural communities are often poorer than those who live in urban areas, which means they’re less likely to have health care coverage from a private insurer. Doctors are reimbursed at lower rates with Medicaid, causing doctors to have trouble making as much money in rural areas. That’s why some doctors leave or accept fewer patients that don’t have private insurance.
If a doctor stays in a rural area and is the only OB-GYN in the area, the doctor could end up with more work than desired.
“One doctor I spoke with for this piece talked about how if you’re the only OB-GYN doctor in the area, obviously you can’t predict when women are going to go into labor, so you would potentially be fielding a lot of calls and be on the road driving to a lot of different places,” Maron said
Another cause of the maternal health care problem is how expensive obstetrics is. The health editor said studies have found obstetrics-gynecology accounts for more than 5 percent of hospital costs. Part of that cost is the unknown factor of how long it will take to deliver a baby. The number of nurses, doctors, surgeons and anesthesiologists who need to be around during that time can add up.
These issues don’t just affect OB-GYN doctors — they affect nurses and midwives, too, and these professionals are moving out of rural areas as well.
“Rural communities in general are graying, it’s a demographic fact that reduces the number of births and makes it difficult for a midwife, just like a hospital, to financially justify living in the area,” Maron said.
There are a couple possible solutions. Maron said that until now there have been tracts within existing medical programs where a doctor might do a rotation in a rural area during his or her residency. But the University of Wisconsin School of Medicine and Public Health is launching the nation’s first official obstetrics gynecology residential program to help address the shortage of OB-GYNs in rural areas. The program will select one resident who will have rotations in hospitals and clinics across the state.
“But when I say resident, note that that’s singular. And their program for very rural areas is just starting with one resident. Obviously that isn’t a large enough fix to try to look at these issues more broadly, but it is a start,” Maron said.
The thought behind this program is that where doctors train is statistically where they’re more likely to practice long term. The hope is that if you train more doctors in rural areas, they’ll stay.
-
In Rural America, Maternal Health Care Services Getting Harder To Find
In rural parts of America, maternal health care services are getting harder to come by. Why? A health and medicine reporter looks at the reasons behind the decline, and what it means for the health of women and their babies.
-
Job Loss, Identity, And Mental Health
The loss of a job can be scary. For many people, unemployment brings uncertainty about how to pay bills or cover costs for basic needs. We talk to an expert who says there’s another important aspect of job loss to pay attention to — the psychological impact, particularly how it affects a person’s mental health and identity.
Episode Credits
- Veronica Rueckert Host
- Judith Siers-Poisson Host
- Amanda Magnus Producer
- Chris Malina Producer
- Haleema Shah Producer
- Katelyn Ferral Guest
- Dina Fine Maron Guest
- Dawn R. Norris Guest
Wisconsin Public Radio, © Copyright 2025, Board of Regents of the University of Wisconsin System and Wisconsin Educational Communications Board.