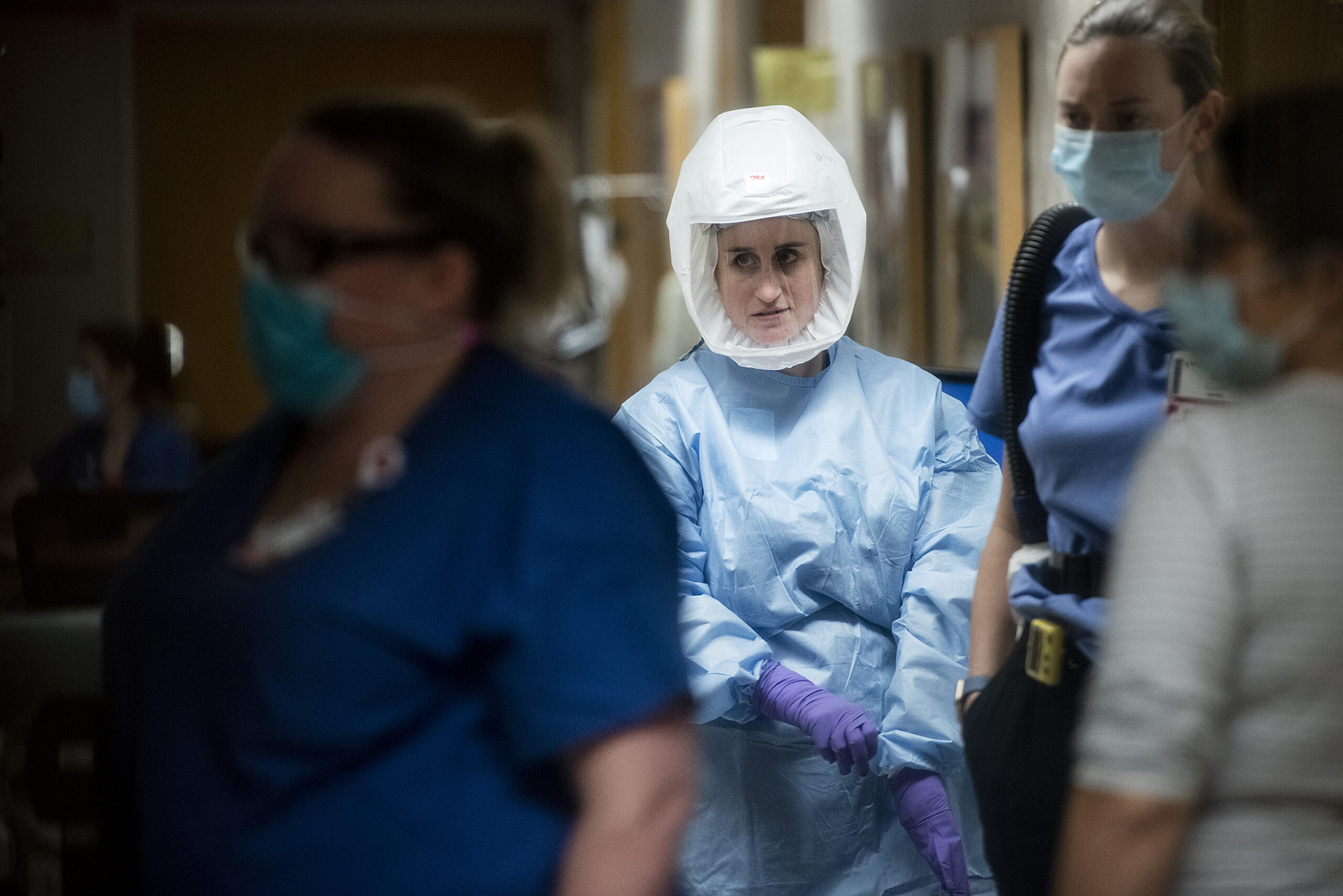
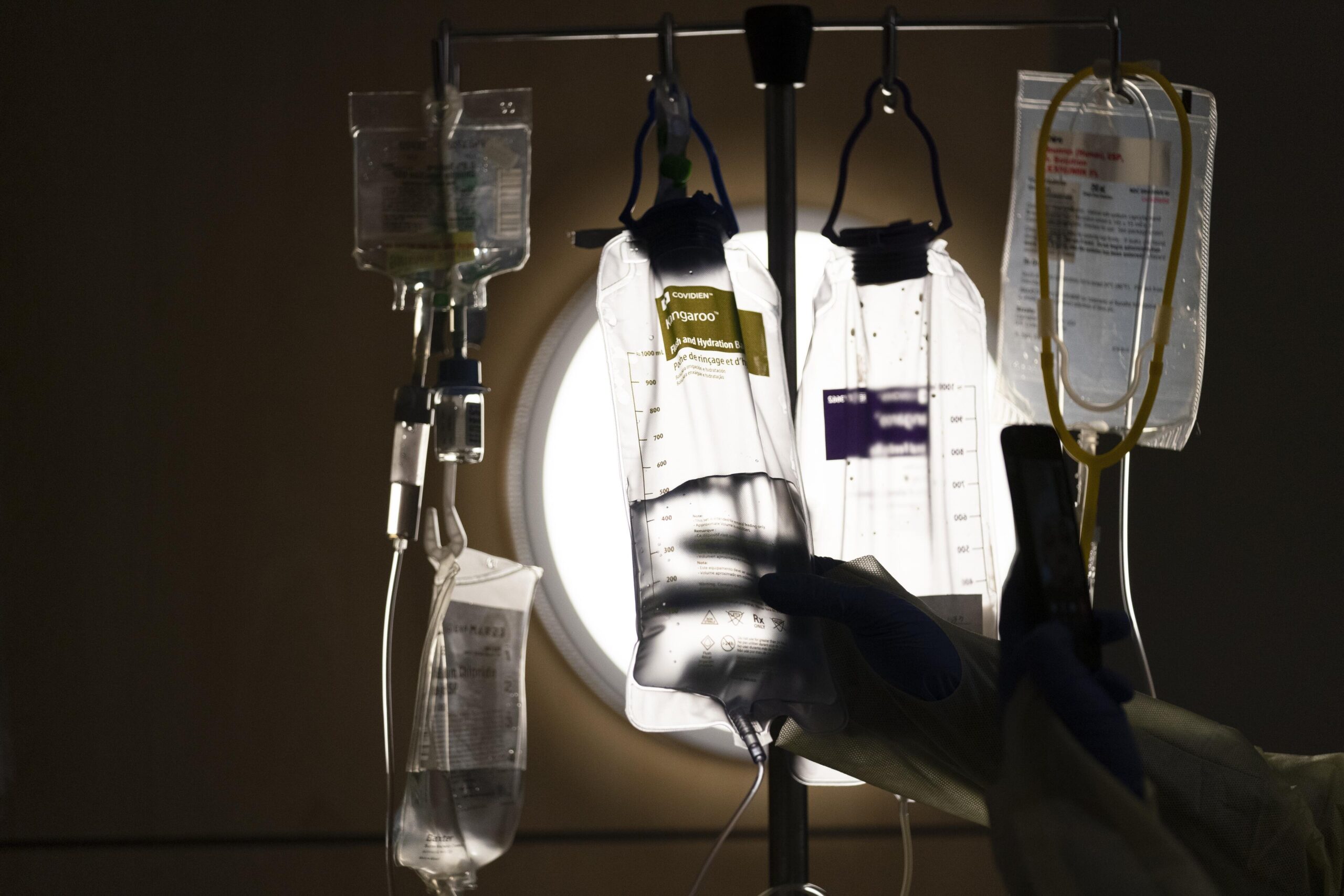
Day in and day out since March, intensive care unit nurse Laura Roth has taken care of COVID-19 patients at a hospital in the Milwaukee area. Roth has watched colleagues get so disheartened by the experience that they request transfers, or leave the profession entirely.
Nurses and medical professionals around the state and country are burning out and running on empty as the pandemic continues to surge and hospitals are overwhelmed with patients. Public health officials warn this winter could be the most difficult time in the nation’s public health history.
“It’s a marathon you’ve had to run, thinking it was going to be a sprint,” Roth said. “We’re short on nurses — we were before the pandemic — and now things are stretched more thin. Every day you go to work and it’s a threat of getting mandated for 16 hours, or taking a number of patients to your assignment that you’re uncomfortable with.”
News with a little more humanity
WPR’s “Wisconsin Today” newsletter keeps you connected to the state you love without feeling overwhelmed. No paywall. No agenda. No corporate filter.
As of Tuesday, 1,556 people are currently hospitalized in Wisconsin with COVID-19, according to the Wisconsin Hospital Association.
While the number of cases in Wisconsin has declined over the last couple of weeks, experts caution that may just be a blip before another surge.
COVID-19 is a minute by minute disease, said Heather Schimmers, the chief nursing officer for Ascension Wisconsin. As the disease progresses, a patient’s status can change almost immediately, requiring a transfer to the ICU.
And as hospital staff get sick or exposed, staffing has also become minute by minute. Schimmers compared managing staffing and beds to playing a game of chess every day.
In Roth’s hospital system, over 200 employees are currently out because they either have COVID-19 or have been exposed.
Pre-pandemic, Roth would take care of just one ICU patient at a time if they were being treated for something that needed to be kept under close watch, such as continuous dialysis or recovering from heart surgery. ICU nurses would max out at two patients at a time.
Recently, she had three ICU patients at once.
“In the ICU, you kind of have to have eyes on your people at all times,” Roth said. “Just knowing that there’s a possibility that you can’t do that, it just makes you feel vulnerable for mistakes, vulnerable to fall short and not do the best nursing that we all want to do.”
If a nurse needs to care for more patients than is standard, Roth said a certified nursing assistant or someone from a different department — that you’re likely not used to working with — may be assigned to help.
“Maybe we get our job done and we deliver our meds on time … but then there’s not room for other things that matter a lot as well, like tending to their mental health, putting extra time to help rehabilitate them physically,” she said. “It just makes you feel like you’re unable to do your best job that you’d like to do.”

To deal with staffing shortages at Bellin Health in Green Bay, COO Sharla Baenen said they’ve redeployed over 250 staff members, had staff come out of retirement, and relied on traveling nurses, among other creative solutions.
But it’s not enough, said Schimmers, whose hospital system has turned to similar solutions.
One of the hardest parts to come to terms with, Roth said, is how preventable so many of the infections could have been.
“Hearing all their stories and knowing how easily, easily prevented it could have been, and then maybe watching them die a few days later, it’s just stunning,” she said. “You hear a story of, ‘Oh, I went out to Friday fish fry.’ And, you know, that person never walks out of the hospital.”
After every shift, Roth said she comes home and “spills her guts” to her fiance in an attempt to process what she’s seen. It frustrates her that the virus continues to spread and people ignore public health pleas to wear a mask, wash your hands and stay home. But people think it isn’t going to happen to them, she said.
Like Nothing They’ve Ever Seen
Over 3,800 people have died of COVID-19 in Wisconsin since March. COVID-19 is an isolating disease. When loved ones can’t visit, it’s the nurses and medical professionals that are there holding patients’ hands, Schimmers said — but it’s difficult to pour from an empty cup.
“We are called to serve, but this is not what we signed up for. I’ve heard many a time the comment, ‘Well, people that work in health care, this is what you signed up to do,’” she said. “This is very different.”
Roth has worked as an ICU nurse for years. Difficult situations are nothing new to her. But this is unlike anything she’s ever seen.
“It’s hard watching people deteriorate from this illness so quickly,” she said. “Oftentimes, people don’t quite understand it and some people don’t believe that it’s even happening. They don’t want to wear their oxygen or they don’t want to accept medicines we’re trying to give them … that can be really hard.”
It has made her question why she decided to become a nurse, and has left her more jaded about the profession than ever before. Working hard to keep people healthy — at great personal risk — when safety guidelines are ignored takes a toll, she said.
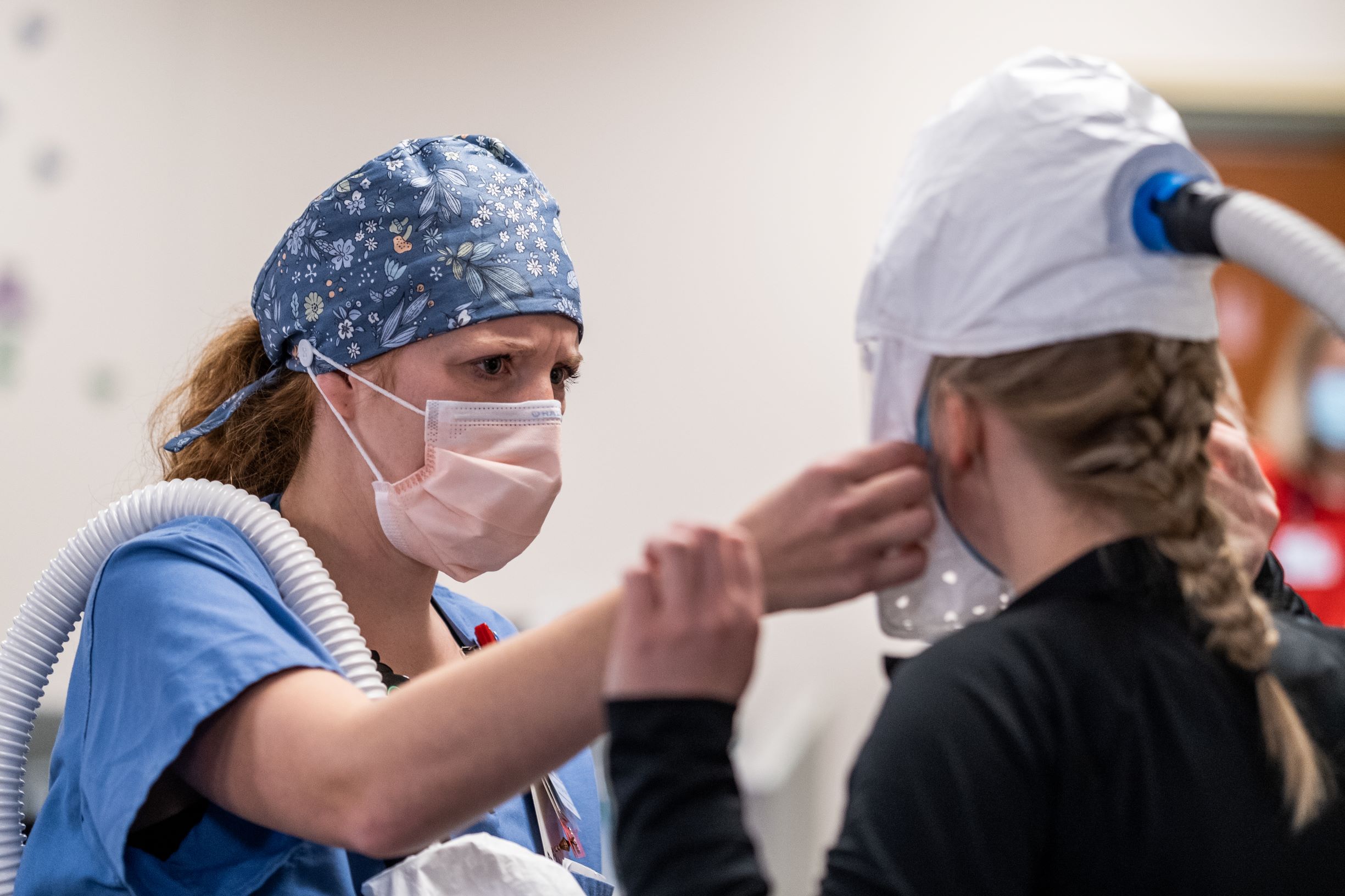
Hospital administrators are trying to do what they can to alleviate some of the pressure and stress, but resources are limited and there isn’t time during a shift to take a break, Roth said.
“Throughout the whole pandemic, I’m just kind of screaming in my head, ‘Why isn’t the government doing something more? Why don’t people believe this?‘” she said.
“It’s hard to hear all the ‘Thank you, health care workers,’ get the pat on the back, but it feels a little patronizing when there’s such a lack of support and such a lack of seeing our community actually follow through with these measures,” Roth said.
With vaccines potentially beginning to reach health care workers in the coming weeks, there is light at the end of the tunnel. But both Roth and Schimmers are worried what Thanksgiving and the upcoming holiday season will mean for case counts.
“If we just take this year off to see your family at the holidays, just try to hang in there a little bit longer,” Roth said. “We can see it with the vaccines coming out, we just need to hang in there and keep going.”
That’s what Roth plans to do: Keep going. In the spring, she’ll begin pursuing her Master’s degree in nursing, in the hopes that on the other side of the pandemic there will be a greater emphasis on health care education.
Wisconsin Public Radio, © Copyright 2026, Board of Regents of the University of Wisconsin System and Wisconsin Educational Communications Board.