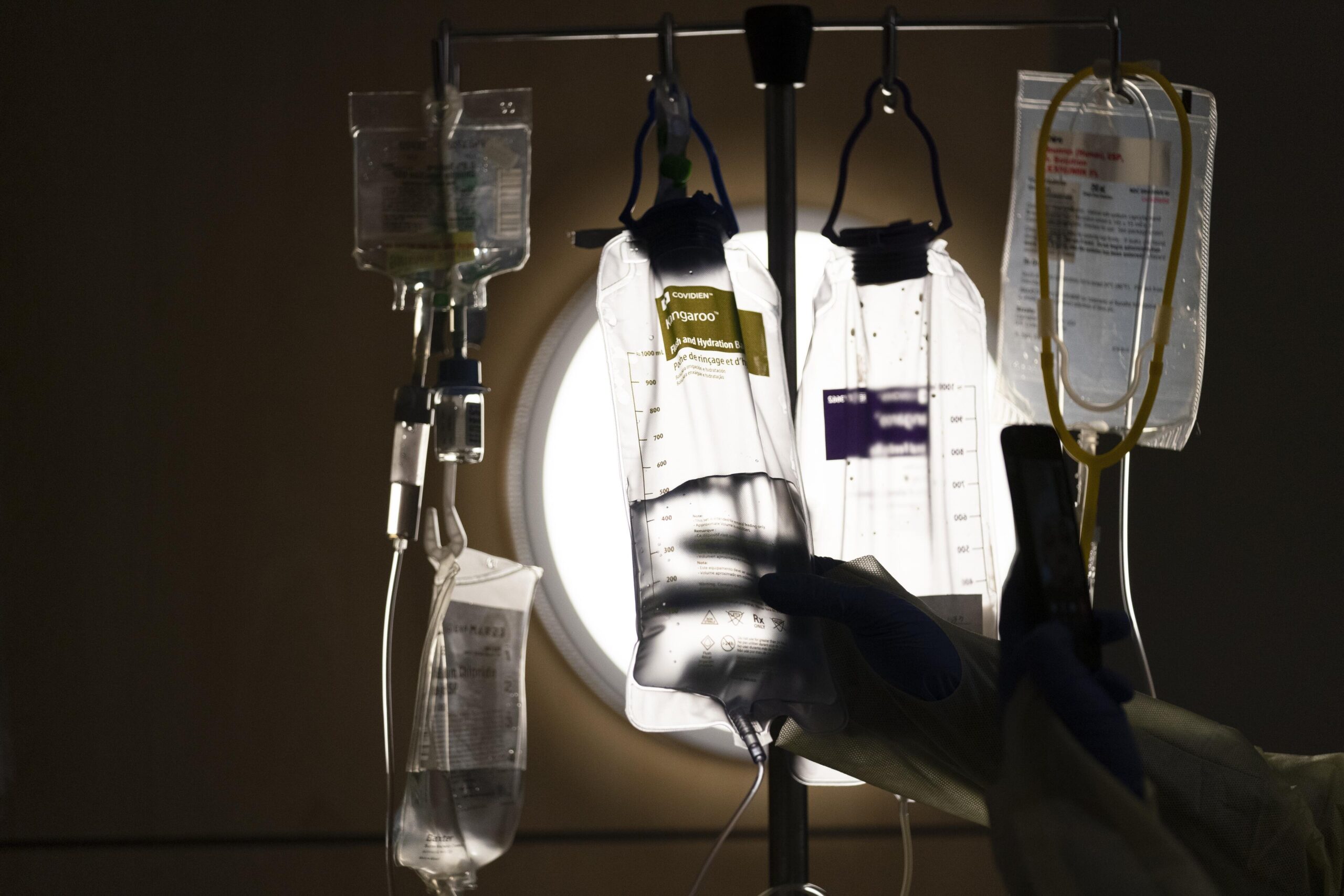
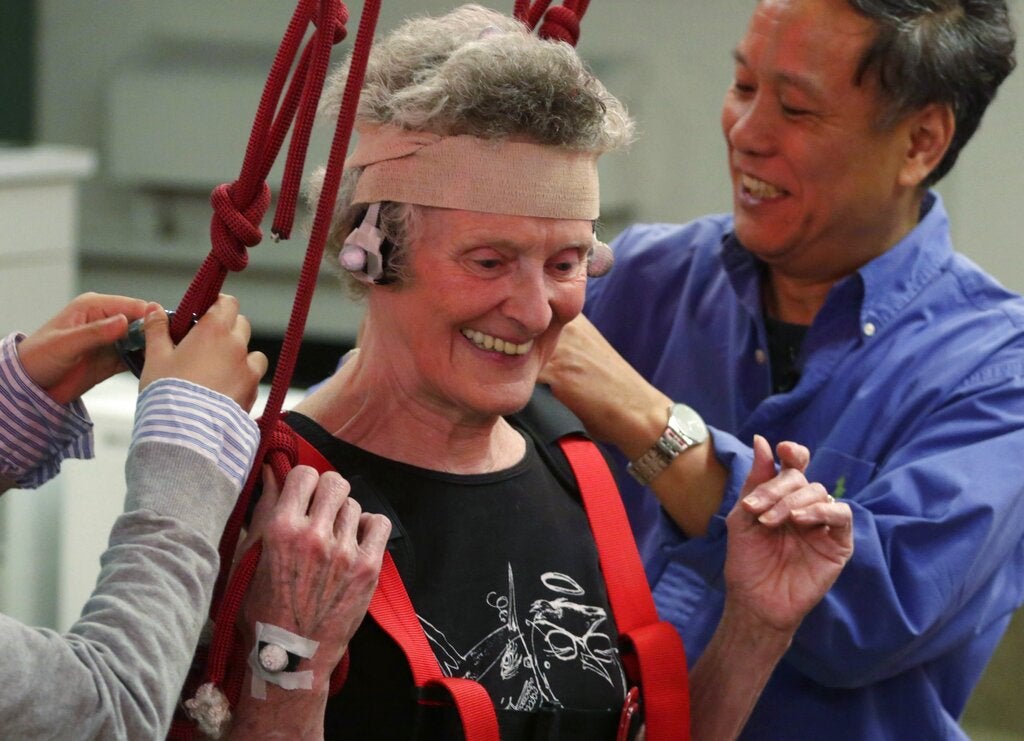
State authorities and the University of Wisconsin-Green Bay are seeking to train 10,000 people this year as certified direct care professionals with a new online program.
The $1.85 million program is free to participants and is being funded mostly by federal aid, according to the Wisconsin Department of Health Services. The agency says the state’s caregiver workforce is in “crisis” and 20,000 more caregivers are needed by next year.
Two health department officials overseeing the new program recently joined Wisconsin Public Radio’s “The Morning Show” to discuss the effort. Jamie Kuhn is the agency’s Medicaid director and Kevin Coughlin is a policy advisor for Medicaid services.
News with a little more humanity
WPR’s “Wisconsin Today” newsletter keeps you connected to the state you love without feeling overwhelmed. No paywall. No agenda. No corporate filter.
Coughlin said more than 2,000 individuals had signed up for the program. Kuhn said the agency is seeking to train “as many individuals as we can.”
The following was edited for clarity and brevity.
Kate Archer Kent: Why set a goal of training 10,000 people as certified direct care professionals?
Jamie Kuhn: We have to set a goal, and we want to try to train as many individuals as we can. If we exceed that goal, that also would be equally exciting. But we also know that if we’re going to make sure our residents stay healthy and safe, that we are going to need to support our caregivers who are working directly with our families and the community.
KAK: How does this free training program work?
Kevin Coughlin: It’s fully accessible via online learning. Our partner, UW-Green Bay, has really done a great job of putting together a curriculum that will give the individual the broad skills to work with people with disabilities or our elderly individuals to keep them living their best life in their own homes — in their community.
It’s 14 different competencies that they’ll learn. The nice part is that with that being online, anybody in the state will have access to it, and it’s on demand so that they can do it at their own pace. We’re just there to help support them through this education journey of theirs. Then, once they complete it, they take a proctored online virtual exam and they then go on our registry.
KAK: Can a digital certification training program adequately prepare people for a real hands-on environment?
KC: We did a lot of research on this, and we’ve learned a lot during the pandemic and especially at the UW-Green Bay. They’re really experts in curriculum development and giving training out to individuals. They put in place a lot of different techniques to make it more of an almost one-on-one experience as they’re taking their training. But this training is not everything that they’re going to need.
The providers and agencies that they work for are also going to have to provide additional support and training. Then we have another part of our scope of work where our certification will be linking to other microcredentials. Those microcredentials might be additional training that will get a little bit more in-depth on the skills that they need as they’re out in those community placements.
READ MORE: Wisconsin health care groups say new state budget helps address workforce shortage
KAK: The new online certification program does include a $500 bonus for people who become certified and stay employed for six months. Are bonuses currently incentivizing people to sign up?
KC: Our program just started in the middle of July, so we already have over 2,000 individuals that have signed up, and they’re ready to start their new career. In 2018, we had a very similar project to get people to work in nursing homes. What we’ve heard from many caregivers is that it wasn’t everything, but it was a very big thing for them.
KAK: Eighty-eight percent of Americans prefer at-home assistance over nursing homes. That is according to a survey in 2021 by the Associated Press and the Center for Public Affairs Research. Is demand for at-home caregivers growing here in Wisconsin?
JK: I think, unequivocally, yes, we are. As the population continues to age, we know that this is an important priority for individuals in Wisconsin and across the country. We are working really hard on many, many initiatives related to providing services for individuals in their home and in their community. It will continue to grow, and we will need to be innovative in this space.
We are very fortunate that we were able to use American Rescue Plan dollars to support a number of initiatives in this space where we are working to support people through home and community-based services. This program also is not just for individuals who are receiving that care through Medicaid but also in the private sector.
We are collaborating with many partners and that’s what it’s going to take. As we see an increase in the need, we’re going to continue to need to collaborate. This program is really the epitome of how collaboration can work throughout the state to ensure that we are recruiting more individuals to care for our family members.
READ MORE: Wisconsin health department introduces new independent living pilot program
KAK: How effective is this type of program model to address the workforce shortage of caregivers?
KC: We’re seeing it as a very successful model. I think other states are looking at Wisconsin. I was recently at a national conference for home- and community-based services. We were featured on three different panels because of some of the innovation that we’re doing here in Wisconsin related to the workforce.
Everybody’s scratching their head trying to figure out what we do. I think we’re really taking a comprehensive approach to this. We have lots of partners. We’re working with the Department of Public Instruction, the Department Workforce Development, with youth apprenticeship programs and career pathways for young high school kids to think about this as a career.
KAK: The Family Care program and the Medicaid long-term care program are receiving $89 million in funds to raise wages for both personal care workers and direct care workers. What do you hope this effort accomplishes?
JK: We know that the work that direct care providers do is invaluable. We agree that they should be able to make a living and provide this compassionate, intimate service that the need is just going to increase. We hope that it will show anyone that is interested in the profession that the administration is supportive of the work they do, and we will continue to work hard to address their wages and value that work.
READ MORE: Wisconsin’s elder care facilities face staffing, financial challenges that threaten care
Wisconsin Public Radio, © Copyright 2026, Board of Regents of the University of Wisconsin System and Wisconsin Educational Communications Board.